CVD is a leading cause of death(1, Reference Miniño, Murphy and Xu2) and this is also so among African Americans(Reference Yusuf, Reddy and Ôunpuu3). Among non-Hispanic blacks aged 20 years and older, 46 % suffer from CVD(4), and CVD caused the deaths of nearly 100 000 African Americans in 2012. CVD risk factors such as age and gender are non-modifiable, while smoking, blood pressure (BP), diabetes, blood lipids and obesity, particularly waist size, can be modified. Of these, hypertension may be most important(Reference Kannel5), particularly considering its high prevalence in this group(Reference Watson6).
A substantial body of evidence has shown that diet plays a role in the pathogenesis of cardiovascular risk factors. Hypertension, for example, can sometimes be controlled by diet alone as verified by the DASH (Dietary Approaches to Stop Hypertension) diet(Reference Moore, Conlin and Ard7), which is rich in fruits, vegetables and low-fat dairy foods, and significantly lowers BP. The mechanism of diet's effect on CVD risk factors is complex. Evidence available from a number of studies links several nutrients, minerals, food groups and dietary patterns with an increased or decreased risk of CVD. Dietary trans and saturated fats, for example, are associated with increased risk of CVD most likely because they increase blood cholesterol(Reference Willett8), while polyunsaturated fats reduce blood cholesterol and appear to be protective(Reference Iacono, Marshall and Dougherty9–Reference Oliver11). Dietary Na is associated with higher BP, while dietary K, well represented in fruits and vegetables, has been associated with reduced risk of hypertension, CHD and stroke(Reference Srinath Reddy and Katan12).
Americans subscribe to a variety of diets aside from the standard American diet. These include the Mediterranean diet and various vegetarian diets such as lacto-ovo-vegetarian, pesco-vegetarian and less commonly the vegan diet which excludes all animal products. Research suggests that a Mediterranean diet is protective for CVD(Reference Williams, Lovegrove and Griffin13). Other studies have shown that vegetarians also have lower BP values and lower risk of CHD(Reference Pettersen, Anousheh and Fan14, Reference Fraser15). In addition, vegetarian diets probably lower rates of diabetes mellitus(Reference Tonstad, Stewart and Oda16) and the prevalence of obesity(Reference Fraser17). Researchers attribute these benefits to less cholesterol and saturated fat in the vegetarian diet, also to the higher content of unsaturated fats, fibre and K(Reference Craig18, Reference Armstrong, van Merwyk and Coates19) and that these diets contain more foods with a lower glycaemic index.
However, much less evidence exists for the health effects of vegetarian diets among African Americans. Studies by Melby et al. have suggested that African-American vegetarians exhibit a more favourable serum lipid profile and also lower BP values than non-vegetarians(Reference Melby, Toohey and Cebrick20, Reference Melby, Goldflies and Toohey21). Studies conducted in Nigeria among native African Seventh-day Adventists demonstrated that the vegetarian diet in this setting also is associated with lower levels of serum total cholesterol (TC), TAG and perhaps BP(Reference Famodu, Osilesi and Makinde22, Reference Famodu, Osilesi and Makinde23).
The African-American diet is typically rich in both fats and complex carbohydrates(Reference Kulkarni24). Obesity is highly prevalent, as 44 % of non-Hispanic blacks have BMI above 30 kg/m2(Reference Flegal, Carroll and Ogden25). In addition, according to estimates in 2011, the prevalence of diabetes is 53 % above the national average in black individuals(26). We therefore conducted a study in blacks (75 % African American and 25 % West Indian) attending Adventist churches in the USA and Canada. Clinics were conducted to measure BP, blood lipids, blood glucose, waist circumference (WC) and BMI. The objective of the present report is to test the hypotheses that there are associations between the identified cardiovascular/metabolic risk factors and different dietary patterns among black individuals.
Experimental methods
Four hundred and seven black women and 185 black men were selected for the present study, which is nested within the Adventist Health Study-2 (AHS-2) cohort. Specifically, these black individuals were those enrolled in the AHS-2 calibration sub-study (n 427) and the Biophysical Manifestations of Religion sub-study (BioMRS, n 165). All individuals were also part of AHS-2. The sub-studies were joined to increase numbers of black participants. The detailed recruitment methods of the AHS-2, the calibration study, the particular methods used to recruit black participants and the BioMRS are described elsewhere(Reference Butler, Fraser and Beeson27–Reference Lee, Morton and Walters30). Briefly, the calibration sub-study participants were representative of all black individuals in AHS-2, and thus were aged 30 years and above, and lived throughout the USA and Canada. Participants from the BioMRS clinics however, lived in Southern California and were at least 50 years of age.
At the clinics, an overnight fasting blood sample, an overnight urine collection and a subcutaneous adipose sample were collected. Biometrics, percentage of body fat (bio-impedence), BP, lipid profiles and selected metabolic parameters were measured using defined protocols. BP was measured while seated and after resting for at least 10 min, using an Omron automated sphygmomanometer(Reference O'Brien, Mee and Atkins31). Systolic BP and diastolic BP were estimated three times 1–2 min apart and the second and third readings were averaged. Lipid profiles – TC (mg/dl), HDL-cholesterol (HDL-C; mg/dl), TAG (mg/dl) and the ratio TC:HDL-C – were measured from fasting blood samples collected in heparin tubes, using a Cholesterol LDX Analyzer (Cholestech Corp., Hayward, CA, USA). LDL-cholesterol (LDL-C) was calculated using the Freidewald equation (TC minus HDL-C minus very-low-density lipoprotein-cholesterol (estimated as TAG divided by 5)) when TAG was <400 mg/dl. The two participants with TAG >400 mg/dl were excluded from this analysis. Weight was determined using the scale function of the Tanita BF-350 Body Fat Analyzer (Tanita UK Ltd, Middlesex, UK). Height was measured using a portable stadiometer, and then BMI was calculated as [weight (kg)]/[height (m)]2. The circumferences of waist and hip were measured using a tape, and their ratio was calculated.
Participants in the BioMRS completed the baseline AHS-2 FFQ within 2–3 years before their clinic visit. Those in the calibration sub-study completed an identical FFQ within 2–3 months of the clinic visit. These FFQ were used to define the dietary patterns. Details of these questionnaires and their use to define the dietary patterns are given elsewhere(Reference Fraser17, Reference Jaceldo-Siegl, Sharma and Knutsen32). Briefly, the dietary patterns are: (i) vegans, who eat no animal products; (ii) lacto-ovo-vegetarians, who eat dairy and/or eggs but no meat; (iii) pesco-vegetarians, who eat fish but no other meats; and (iv) non-vegetarians who eat meats at least once per week.
Physical activity was assessed as hours spent per day in moderate, vigorous and extremely vigorous activities. These were based on questions that gave examples of such activities, including work and leisure exercise, and separated weekdays from weekend days.
Data analysis
The odds ratios of prevalent hypertension, diabetes, larger WC and high lipid levels, comparing dietary patterns, were estimated by the use of logistic regression. Hypertension was defined as any participant with systolic BP ≥140 mmHg or diastolic BP ≥90 mmHg or taking BP-lowering medications; elevated TC (or LDL-C) was defined as values ≥200 mg/dl (or ≥130 mg/dl for LDL-C) or taking lipid-lowering agents; low HDL-C was defined as values <40 mg/ml (males) or <50 mg/dl (females); elevated TAG was defined as values ≥150 mg/dl; diabetes was defined as fasting plasma glucose ≥126 mg/dl or taking diabetic medications. Covariates always included an indicator variable specifying which sub-study an individual came from. The identity of medications used by study participants and which are commonly used to treat hypertension, hyperlipidaemia or diabetes was determined by a cardiologist and internist (G.F.).
Adjusted mean levels of each risk factor by dietary pattern among participants not taking medications for the medical condition or associated risk factor under consideration were calculated from ANCOVA, adjusting for age, gender, education, physical activity and an indicator variable for sub-study. In separate analyses adjustment was also made for BMI. Small percentages of missing data (3–7 %) for individual dietary variables used to establish dietary patterns were imputed as described elsewhere(Reference Pettersen, Anousheh and Fan14, Reference Fraser and Yan33).
Statistical analyses were performed using the SAS statistical software package version 9·3.
Results
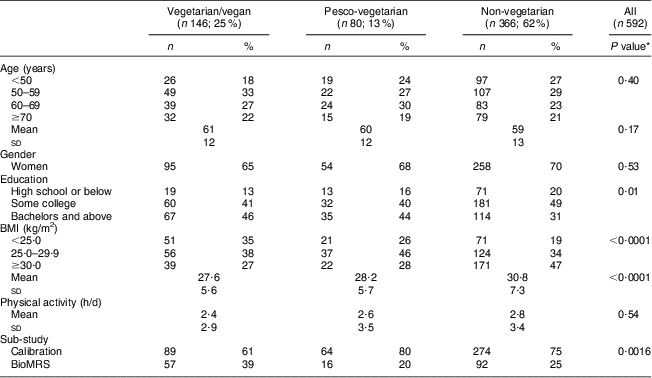
The baseline demographics of the 592 participants, stratified by dietary pattern, are summarized in Table 1. In the combined data, fifty-one participants were vegans, ninety-five lacto-ovo-vegetarians, eighty pesco-vegetarians and 366 were non-vegetarians. We further combined vegans and lacto-ovo-vegetarians because of the small vegan population and because in nearly all dietary respects Adventist lacto-ovo-vegetarians fall between vegans and non-vegetarians(Reference Rizzo, Jaceldo-Siegl and Sabate34). The new category is referred to as ‘vegetarian/vegans’. Non-vegetarians tended to be less educated and to have higher BMI than participants with other dietary patterns (Table 1).
Table 1 Relationship of selected demographic factors to dietary patterns among black participants in the Adventist Health Study-2 (AHS-2)

BioMRS, Biophysical Manifestations of Religion sub-study.
*P values test differences between means of dietary patterns or the null hypotheses of no association between the named variable and dietary pattern.
Apart from age (P < 0·0001), which is a consequence of the design of the two sub-studies (as is probably true also for educational status, P < 0·0001), there were no statistically significant differences in covariate values between the two sub-study groups. Therefore, all subsequent analyses were adjusted for age and education, as well as gender and sub-study indicator variable. The BioMRS participants were, however, more likely to be vegan and less likely to be pesco-vegetarian than the calibration sub-study participants.
Hypertension and diet
Of the 592 participants, 305 were classified as hypertensive and 212 of these were taking anti-hypertensive medications. In multiple logistic regression analysis (Table 2), the vegetarian/vegan group had a significantly lower odds of hypertension compared with non-vegetarians (OR = 0·56, P = 0·01). Results for pesco-vegetarians did not differ significantly from either of the other groups. When restricting the analysis to all participants not taking anti-hypertensive medications (Table 3), adjusted mean systolic and diastolic BP values were on average 1·3 and 0·6 mmHg (P = 0·57 and 0·67) lower, respectively, in vegetarian/vegans than in non-vegetarians. Values for pesco-vegetarians not taking anti-hypertensive medications were higher than those for vegetarian/vegans (P = 0·25) and non-vegetarians (P = 0·43).
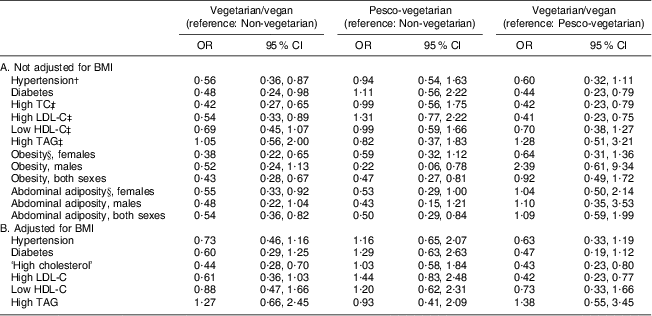
Table 2 Multiple logistic regression analyses to test associations between major cardiovascular risk factors and dietary patternsFootnote * among black participants in the Adventist Health Study-2 (AHS-2)

TC, total cholesterol; LDL-C, LDL-cholesterol; HDL-C, HDL-cholesterol; BP, blood pressure; WC, waist circumference.
* A separate logistic regression model was run for each risk factor, in each case adjusted for age, gender (as appropriate), education, physical activity, sub-study indicator and BMI as indicated.
†Hypertension is systolic BP ≥ 140 mmHg and/or diastolic BP ≥ 90 mmHg or taking medications for high BP.
‡High TC is ≥200 mg/dl and high LDL-C is ≥130 mg/dl or taking cholesterol-lowering medications in either case; low HDL-C is <40 mg/dl (males) or <50 mg/dl (females); high TAG is >150 mg/dl.
§Obesity is BMI ≥ 30·0 kg/m2; abdominal adiposity is WC >88 cm in females and >102 in males.
Table 3 Adjusted mean levels of risk factorsFootnote * among black participants in the Adventist Health Study-2 (AHS-2)

BP, blood pressure; TC, total cholesterol; LDL-C, LDL-cholesterol; WC, waist circumference; HDL-C, HDL-cholesterol.
* Among participants not on medication for that particular risk factor (applies to hypertension, diabetes and lipids), adjusted for age, gender (as appropriate), education, sub-study indicator, physical activity and BMI as indicated.
†P values test the null hypotheses of no difference between the pairs of dietary groups indicated.
Diabetes and diet
Of 592 participants, eighty-five were classified as diabetic and fifty-six of these were taking diabetic medications. The prevalence of diabetes was 8·9 % in vegetarian/vegans, 18·8 % in pesco-vegetarians and 15·6 % in non-vegetarians. Vegetarian/vegan diets were associated with a lower risk of diabetes compared with non-vegetarians (OR = 0·48, P = 0·04; Table 2). Of all vegetarian/vegans who were not taking anti-diabetic medications, the average adjusted fasting plasma glucose level was 7·3 mg/dl lower (P = 0·0003) than that of non-vegetarians (Table 3). Pesco-vegetarians were not significantly different in odds ratio of prevalent diabetes when compared with either vegetarian/vegan or non-vegetarian groups, but those not on medication had higher glucose levels than vegetarian/vegans (P = 0·004).
Serum total cholesterol and diet
Of vegetarian/vegan participants, 30 % were classified as having ‘high cholesterol’ compared with 48 % in both the pesco- and non-vegetarian groups. The odds ratio for high cholesterol in the vegetarian/vegan group, as compared with the non-vegetarians, was 0·42 (P = 0·0001), and a similar value was observed when comparing to pesco-vegetarians (OR = 0·42, P = 0·006; Table 2). Vegetarian/vegans who were not taking cholesterol-lowering medications had an average adjusted fasting plasma TC level that was 10·0 mg/dl lower (P = 0·01) than that in equivalent non-vegetarians (Table 3). Levels in pesco-vegetarians did not differ significantly from those in non-vegetarians.
Serum LDL-cholesterol and diet
In the vegetarian/vegan group 28 % of participants met the criteria for high LDL-C, but 48 % of pesco-vegetarians and 43 % of non-vegetarians were classified in the high LDL-C category. Thus, vegetarian/vegans had a significantly lower odds of high LDL-C compared with non-vegetarians (OR = 0·54, P = 0·015), and a significantly lower odds was also observed when comparing them to pesco-vegetarians (OR = 0·41, P = 0·003; Table 2). Vegetarian/vegans who were not taking cholesterol-lowering medications had on average a 9·6 mg/dl (P = 0·014) lower adjusted mean fasting plasma LDL-C level compared with equivalent non-vegetarians (Table 3). Levels in pesco-vegetarians did not differ significantly from those in non-vegetarians.
Serum HDL-cholesterol and TAG
In these analyses we did not observe any significant differences in fasting plasma levels of HDL-C or TAG among dietary patterns (Tables 2 and 3).
BMI, waist circumference and diet
Results are computed separately for males and females as we found that the average BMI in females was significantly higher than that of males. The odds ratios for obesity (BMI ≥ 30·0 kg/m2) and abdominal adiposity (WC >88 cm in females and >102 cm in males) are shown in Table 2. Those for obesity are 0·38 (females, P = 0·0005) and 0·52 (males, P = 0·10) comparing vegetarian/vegans with non-vegetarians. Corresponding odds for abdominal adiposity are 0·55 (P = 0·02) and 0·48 (P = 0·06). Thus similar trends in both sexes were noted by dietary pattern except that the point estimates for the pesco-vegetarian males were non-significantly lower than those for vegetarian/vegans.
Adjusted mean BMI and WC data for each dietary pattern are shown in Table 3. Both mean BMI and WC were significantly associated with the vegetarian dietary patterns. A trend of increasing BMI was noted passing from vegetarian/vegan, to pesco-vegetarian, to non-vegetarian patterns, the difference between vegetarian/vegan and non-vegetarian being highly significant. This was true for both genders. Values of mean WC were significantly lower in both vegetarian/vegans and pesco-vegetarians compared with non-vegetarian participants. Pesco-vegetarians had significantly lower mean BMI (P = 0·0006) and WC (P = 0·0003) than non-vegetarians, but did not differ significantly from vegetarian/vegans on either the odds ratios or the adjusted means.
Tables 2 and 3 also show results with additional adjustment for BMI. In Table 2 there is usually some moderate movement of the effect estimate towards the null, indicating that differences in BMI according to diet partially mediate the dietary effects. However, dietary effects on TC and LDL-C still retain statistical significance (or very close), suggesting that here diet also acts independently of BMI. In Table 3, among those not taking diabetic or lipid-lowering medications, significant differences remain between dietary patterns for TC, LDL-C and fasting glucose.
Discussion
We found that black vegans and lacto-ovo-vegetarians (as a combined category) had significantly lower prevalences of major CVD risk factors compared with non-vegetarian black Adventists. These results are from a population that includes both genders, a wide age range and a broad span of socio-economic status and location of residence. There is a growing body of evidence about the beneficial effects of vegetarian dietary habits on cardiovascular health among non-black populations, but similar effects have not been extensively studied among black populations. As we have previously reported, black Adventists may have lower rates of CVD than other blacks(Reference Montgomery, Herring and Yancey35). If so, this could be due in part to the sizeable percentage of vegetarians among the Adventists.
As compared with non-vegetarians, vegetarian/vegans had a 44 % lower odds of hypertension, an important finding for black individuals where hypertension is so prevalent. However, there was no significant difference in risk between pesco-vegetarians and non-vegetarians. These results generally agree with those of another study of black Adventists in Nigeria where omnivores had higher systolic BP values than vegetarians, although this was not statistically significant(Reference Famodu, Osilesi and Makinde22). Two studies of African Americans(Reference Melby, Toohey and Cebrick20, Reference Melby, Goldflies and Toohey21) demonstrated significantly lower BP in vegetarians, with the first showing lower systolic pressures (by 10·2 mmHg)(Reference Melby, Goldflies and Toohey21) compared with omnivores and the second study finding similar but non-significant trends(Reference Melby, Toohey and Cebrick20). Among blacks in Barbados who had been vegetarian for at least 5 years there was a lower percentage with self-reported hypertension (although not statistically significant)(Reference Brathwaite, Fraser and Modeste36). The CARDIA (Coronary Artery Risk Development in Young Adults) study(Reference Steffen, Kroenke and Yu37) investigated a cohort with approximately equal numbers of black and white participants. Consistent across race–sex groups the intake of plant foods was inversely associated, while meat was positively associated, with elevated BP. Although analyses were adjusted for race and other factors, it was not stated if this was true separately in black individuals. The DASH diet also lowered BP significantly by 6·9/3·7 mmHg in African Americans(Reference Sacks, Appel and Moore38). This diet has a reduced amount of meat and more fruit, vegetables and whole grains than a typical US diet.
Protective associations between vegetarian diets and high BP are consistent with studies of non-black populations. Several small experimental studies(Reference Sacks, Donner and Castelli39–Reference Margetts, Beilin and Vandongen42) and larger observational studies(Reference Appleby, Davey and Key43), including white participants in AHS-2(Reference Pettersen, Anousheh and Fan14), have generally found similar results to those that we report here in black North Americans. Further, studies of non-vegetarians have often, in multivariate analyses, associated plant foods (such as whole grains, fruits, etc.) with lower BP and meat consumption with higher BP, as recently reviewed by Steffen et al.(Reference Steffen, Kroenke and Yu37).
The mechanisms underlying the effect of vegetarian diets on hypertension are unclear. However, the greater intakes of K, other minerals and fibre in vegetarian diets have been postulated to reduce BP(Reference He and Bazzano44), as have higher intakes of the minerals, Ca, K, Mg and P(Reference Reusser, DiRienzo and Miller45). It is possible that meat appears to increase the risk of hypertension because of its association with fewer vegetables and fruits. As found by others(Reference Appleby, Davey and Key43), it also seems clear in our data that a large part of this effect is related to the lower BMI among vegetarians. Plant foods are also known to protect against insulin resistance which in turn is related to hypertension and other risk factors for heart disease(Reference Lee, Lorenzo and Haffner46).
Our study also found that vegetarian/vegans have less than half the odds of diabetes of non-vegetarian black participants, a potentially important finding for black women particularly, as they had higher glycaemic index and glycaemic load than Caucasians in the SWAN (Study of Women's Health Across the Nation) cohort(Reference Hu, Block and Sternfeld47). In black participants from the parent AHS-2 cohort, Tonstad et al. (Reference Tonstad, Stewart and Oda16) reported in covariate-adjusted analyses that vegans (OR = 0·381; 95 % CI 0·236, 0·617), lacto-ovo-vegetarians (OR = 0·618; 95 % CI 0·503, 0·760) and semi-vegetarians (OR = 0·486, 95 % CI 0·312, 0·755) had a lower self-reported incidence of diabetes than non-vegetarians. A few other cohorts have found that certain foods, often those preferentially consumed by vegetarians, were associated with lower risk of diabetes in black individuals. Analysis of a small cohort of ethnic minority women (half were black) from the Nurses’ Health Study, but with long follow-up, suggested that a healthy diet high in cereal fibre but low in trans fat and glycaemic load was perhaps even more strongly associated with reduced diabetes risk than in white individuals(Reference Shai, Jiang and Manson48). In the 59 000 black women enrolled in the Black Women's Health Study, higher intake of cereal fibre was associated with lower risk, and higher glycaemic index with higher risk of diabetes(Reference Krishnan, Rosenberg and Singer49). The ARIC (Atherosclerosis Risk in Communities) study found a protective association between cereal fibre and diabetes risk in both white and black participants, but this was not statistically significant among the blacks(Reference Stevens, Ahn and Juhaeri50). However, in the CARDIA study (where half of the subjects were black) those following the Dietary Guidelines for Americans had increased insulin resistance compared with others in this population(Reference Zamora, Gordon-Larsen and He51).
Studies of vegetarian diets from other populations, and risk of diabetes in black or non-black individuals, are rare, although much is known of the use of such diets in the treatment and control of diabetes(Reference Barnard, Katcher and Jenkins52). A previous cohort of US Adventists has provided strong positive associations between intake of meat and incidence of diabetes(Reference Vang, Singh and Lee53).
Several mechanisms are postulated for the beneficial effects of the vegetarian diet on diabetes risk. Undoubtedly the most important is the lower rates of overweight associated with these diets, and in our data, the magnitude of the effect is diminished after adjustment for BMI. Vegetarian diets usually also have lower glycaemic load, which is known to decrease risk of diabetes(Reference Barclay, Petocz and McMillan-Price54). Red meats increase insulin resistance, an effect possibly mediated by saturated fats(Reference Bruce, Wolever and Giacca55). In addition, fruit and vegetable intake is associated with reduced oxidative stress and inflammation, possible precursors of diabetes(Reference Romeo, Lee and Shoelson56).
The vegetarian/vegan diet was associated with 9·6 mg/dl lower LDL-C, 10·0 mg/dl lower TC and just over half the risk of elevated LDL-C as found in non-vegetarians. Other studies of effects of vegetarian diets on lipid levels in black populations are rare. Toohey et al. (Reference Toohey, Harris and DeWitt57) found that lipid levels in black vegans were more favourable than those of lacto-ovo-vegetarians in the USA. In our study, because of the small number of vegans, we combined these two dietary patterns. Melby et al. (Reference Melby, Toohey and Cebrick20) found lower TC, LDL-C and TAG among sixty-six black vegetarians compared with forty-five non-vegetarians in the USA. Very similar results were demonstrated by Famodu et al. (Reference Famodu, Osilesi and Makinde22) among black Adventists (vegetarian and non-vegetarian) in Nigeria.
Vegetables are known to decrease TC and LDL-C values(Reference Fraser, Jacobs and Anderson58), while saturated fats significantly increase and polyunsaturated fats lower both serum LDL-C and TC(Reference Jacobs, Anderson and Blackburn59). Dietary fibre and phytosterols, found only in plant foods, also have a well-established but modest effect to lower serum cholesterol(Reference Bazzano60), whereas red meat raises it(Reference Sacks, Donner and Castelli39). Thus there is every reason to expect a more favourable lipid profile among vegetarians, which has usually been found(Reference Ferdowsian and Barnard61–Reference West and Hayes63).
Our results showed that vegetarian/vegans have a risk of obesity that is only 43 % that of non-vegetarian black participants. The risk of abdominal adiposity was similarly much reduced in both vegetarian dietary patterns. These were the only cardiovascular risk factors where pesco-vegetarians seemed to benefit at least as much as the vegetarian/vegans. Brathwaite et al. (Reference Brathwaite, Fraser and Modeste36) demonstrated less obesity among black participants in Barbados who had been vegetarian for at least 5 years. Other studies in black individuals have also found lower BMI and/or waist and hip sizes among vegetarians(Reference Melby, Toohey and Cebrick20–Reference Famodu, Osilesi and Makinde22). The CARDIA study, a cohort consisting of about half black participants, showed strong inverse associations between intake of plant foods and both BMI and WC(Reference Steffen, Kroenke and Yu37). That vegetarians are less overweight has been shown in several non-black research populations(Reference Vang, Singh and Lee53, Reference Berkow and Barnard64, Reference Key and Davey65). The mechanisms are unclear but probably include the higher energy density of meats and characteristics of plant foods that replace them in a vegetarian diet. We adjusted for differences in physical activity in the present study. Differences in energy intake by dietary pattern appear to be small(Reference Rizzo, Jaceldo-Siegl and Sabate34).
Although broadly similar trends are found in Tables 2 and 3, an important difference in Table 3 is that for BP, blood glucose and blood lipids, the results here are limited to those participants who either do not have abnormal values or if they do, are untreated. This is because drug treatment lowers values to an unpredictable extent, perhaps to below normal values in some cases, thus potentially obscuring any dietary effect within the normal range. Even with this exclusion, differences between dietary patterns may be diminished as individuals with more severe abnormality are often excluded. Smaller numbers of participants may also impact statistical significance.
The study has the weakness of being cross-sectional, which does not establish causality. However, most Adventists with health problems will most likely change towards vegetarianism rather than in the opposite direction because of church recommendations on lifestyle. This is indicated by data from AHS-2 (M Martins and GE Fraser, unpublished results) that show strong within-subject trends towards lower animal food intake with ageing. Such dietary changes due to poor health would bias our findings towards the null. A strength of the study is the relatively large sample size of black participants with high-quality dietary data and the careful risk factor assessment.
Conclusion
In summary, we provide evidence that black vegetarians show less hazardous values of several established cardiovascular risk factors when compared with non-vegetarians. This would be expected to translate into reduced risk of heart attack, stroke and renal failure. Being cross-sectional, our results do not prove a causal association with vegetarianism, but provide some evidence for this.
Acknowledgements
Sources of funding: The authors gratefully acknowledge support from the National Institutes of Health (NIH)/National Cancer Institute (NCI; grant # U01CA152939). The NIH/NCI had no role in the design, analysis or writing of this article. Conflict of interest: None of the authors has a conflict of interest to report. Ethics: The study was approved by the Loma Linda University Research Protection Program. Authors’ contributions: G.F. obtained funding, contributed to the study design and wrote part of the manuscript. R.A. performed part of the analysis and reviewed the manuscript. P.H. promoted study enrolment among black individuals, assisted with data collection and reviewed the manuscript. S. Knutsen contributed to the study design, assisted with data collection and reviewed the manuscript. S. Katuli wrote part of the manuscript and reviewed the manuscript. Jing Fan contributed to the data analysis and reviewed the manuscript.