INTRODUCTION
Sparganosis or plerocercoidosis is a parasitic disease caused by the plerocercoid, the third larval stage of diphyllobothroid tapeworms belonging to the genus Spirometra, most commonly Spirometra erinaceieuropaei (also called S. erinacei or S. mansoni) in Asia [Reference Cobbold1, Reference Manson, Manson-Bahr and Wilcocks2] and Spirometra mansonoides in North America [Reference Mueller3]. Adult Spirometra worms parasitize the intestines of dogs and cats, and rarely humans (spirometrosis). The parasites exploit two intermediate hosts during its life-cycle: copepods as the first intermediate hosts, where the procercoid larva develops, and varieties of vertebrates (amphibians, reptiles, birds, mammals) as the second intermediate hosts, where the plerocercoid larva develops. In nature, frogs mainly act as second intermediate hosts, and frog-eating predators, such as snakes and birds, are paratenic hosts [Reference Mueller3]. The parasite is transmitted to humans in three different ways: waterborne (drinking raw water contaminated with copepods carrying procercoids), foodborne (ingesting raw or undercooked meat of the second intermediate hosts or paratenic hosts carrying plerocercoids) and contact (mainly by the application of frog flesh as a poultice in traditional medicine in several countries in Asia) [Reference Cho4, Reference Ausayakhun5].
Plerocercoids can invade subcutaneous tissue/muscle, eyes, brain, urinary tract, pleura, spinal canal and other tissue/organs of the human body, leading to various clinical symptoms according to the location of the parasites within the host [Reference Li6]. Misdiagnoses of sparganosis are rather common and most cases are diagnosed following surgical removal of the worm, especially in cases of infections of the central nervous system (CNS) and visceral organs [Reference Thomas and Lawrence7, Reference Garcia and Bruckner8]. Although immunodiagnostic and CT/MRI methods have been developed, identification of risk factors has significant value for pre-operative diagnosis. Surgical removal of the worms is the best treatment of this disease, in contrast, medication (praziquantel, mebendazole, etc.) has limited success. Prevention strategies should focus on food and water sanitation and against using raw frog or snake flesh as poultices [Reference John and Petri9].
The first human case of sparganosis was reported by Manson in 1882 in China [Reference Manson, Manson-Bahr and Wilcocks2], after that the disease was found widely distributed in many tropical and subtropical countries, especially in East and Southeast Asia. China is one of the main countries to suffer from sparganosis. In the present study, the epidemiology of sparganosis in mainland China from 1959–2012 was analysed.
MATERIALS AND METHODS
The literature relating to sparganosis in China (not including Taiwan, Hong Kong, Macao), from 1959 to December 2012 was collected from online databases including China National Knowledge Infrastructure (CNKI, http://www.cnki.net/), Chinese Medical Current Contents (CMCC), Wanfangdata (http://g.wanfangdata.com.cn/) and other Chinese periodicals using the key words ‘sparganosis’ and ‘plerocercoidosis’. All cases of sparganosis were collected, epidemiological factors such as reporting time, geographical distribution, age and gender of patients, urban/rural distribution, possible risk factors, and tissue/organs involved in each case were extracted to form a table using Microsoft Office Excel 2003; data were analysed by the ratio of percentage (all cases were anonymized for analysis).
RESULTS
Valid cases
Over the period studied, 1114 cases were collected from 411 reports published in 215 periodicals. A total of 52 cases that were repeated in more than one report were excluded. One case that was confirmed as proliferative sparganosis was not included in this study [Reference He and Huang10]. A total of 1061 valid cases accounting for 95·2% of all cases was used in the analysis. Of the valid cases 92·4% (980/1061) were confirmed by pathological observation or direct observation of parasites post-operation, and the remainder (7·6%, 81/1061) were confirmed by immunological diagnostic methods (skin test, ELISA) combined with the patients’ history.
Geographical distribution
Sparganosis was distributed throughout most provinces apart from Inner Mongolia, Shanxi, Tianjin, Gansu, Shaanxi and Tibet (Fig. 1). Nearly 60% of the cases were distributed in the southeast coastal areas (Southern China 31·2%, Eastern China 25·8%). The top five provinces with the highest case load were Guangdong (171), Hunan (112), Hainan (104), Jilin (94), Fujian and Sichuan (89); the top five provinces with the highest incidence were Hainan (1·2), Jilin (0·3), Shanghai (0·2), Fujian (0·2) and Hunan (0·2) according to incidence (1/100 000) calculated from 2012 population data of every province (data not shown).

Fig. 1. Geographical distribution of sparganosis in mainland China.
Sex, age and urban/rural residence of the patients
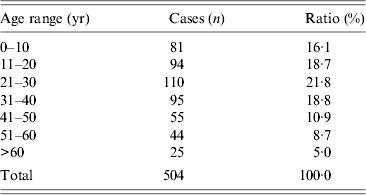
No obvious difference in sex was found (424 male, 465 female) in the 889 cases with gender recorded in all valid cases. Patients’ age ranged from newborn to 80 years in 504 cases with definite age records, the average age was 29 years and most patients were in the 0–50 years age group, accounting for 86·3% (Table 1). Of the 360 cases with occupational records, most patients (74·7%) were from rural areas, with the remainder were from urban areas.
Table 1. Age distribution of 504 cases in mainland China
Tissue/organs and risk factors
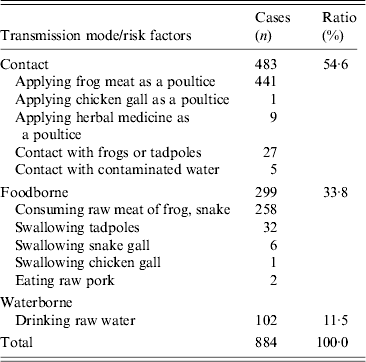
For the 1061 valid cases, the most commonly involved tissue/organs were: subcutaneous/muscles (43·1%), followed by eyes (31·0%), CNS (17·9%), genitourinary system (3·9%), visceral organs (3·2%) and no detailed information recorded (0·9%). Details of the tissue/organs involved are listed in Table 2. In 884 cases with risk factors recorded, the modes of transmission were through contact (54·6%), foodborne (33·8%) and waterborne (11·5%). Details of the risk factors are listed in Table 3.
Table 2. Tissues/organs involved in 1061 cases in mainland China

Table 3. Mode of transmission and risk factors of 884 cases in mainland China
Correlation of the mode of transmission with geographical distribution and tissue/organs
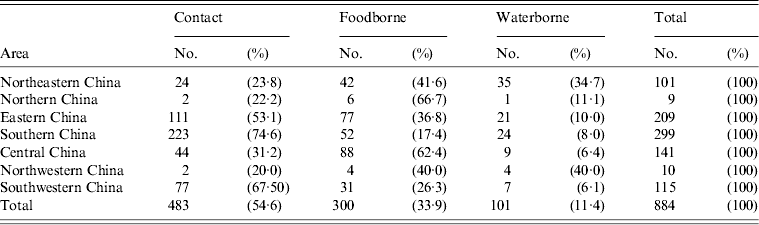
Modes of transmission for the different regions are listed in Table 4. In Northeastern China, Northern China and Central China, the main mode of transmission was foodborne (41·6%, 66·7% and 62·4%, respectively), with most patients having a history of ingesting frog or snake meat. Compared to that, in Eastern China, Southern China and Southwestern China, the main mode of transmission was through contact, especially the application of frog meat as a poultice (53·1%, 74·6% and 67·5%, respectively).
Table 4. Correlation of risk factors with geographical distribution
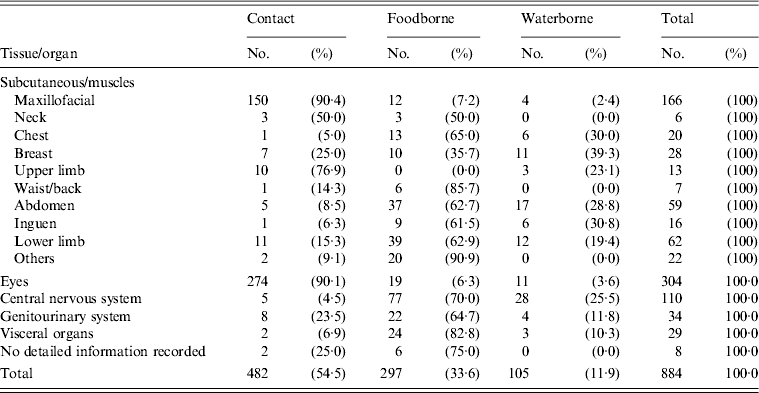
Mode of transmission for cases with the tissue/organs involved is shown in Table 5. For cases of maxillofacial, eye and upper limbs, the main mode of transmission was through contact, mainly the application of frog meat as a poultice (90·4%, 90·1% and 76·9%, respectively). For cases concerning other areas of body, except breast, the main mode of transmission was foodborne, mostly the consumption of raw frog or snake meat.
Table 5. Relationship of mode of transmission with tissue/organs
Tissue/organs and mode of transmission in different periods
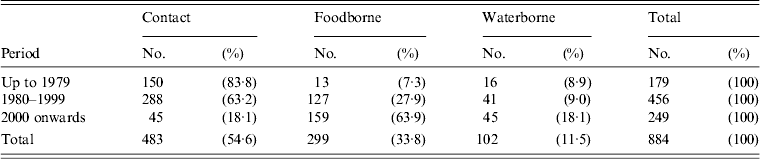
The main tissue/organs involved changed markedly over the period studied. Cases involving eyes decreased from 50·0% pre-1979 to 8·3% post-2000. Cases involving subcutaneous/muscles also exhibited a decrease; while, cases involving CNS and visceral organs increased, especially for CNS, from no case reported pre-1979 to 47·8% post-2000. Most CNS cases (85·3%, 162/190) were reported during this period (Table 6). The main modes of transmission in different periods also changed, cases caused through contact decreased gradually, from 83·8% pre-1979 to 18·1% post-2000; while foodborne cases increased, from 7·3% pre-1979 to 63·9% post-2000; waterborne cases also increased (Table 7).
Table 6. Tissue/organs involved in different periods
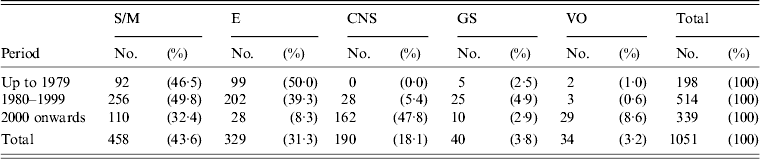
S/M, Subcutaneous/muscles; E, eyes; CNS, central nervous system; GS, genitourinary system; VO, visceral organs; UN, no detailed information recorded.
Table 7. Mode of transmission in different periods
DISCUSSION
There have been more than 1700 global records of sparganosis to date (mainland China, ≈1000 cases [Reference Li6]; Japan, 470 cases [Reference Kimura11]; South Korea, ≈200 cases [Reference Min12]; Thailand, 52 cases [Reference Anantaphruti, Nawa and Vanvanitchai13]). Sparganosis caused by S. erinaceieuropaei is dominant in South and East Asia [Reference Qiu and Qiu14]. A total of 1061 cases analysed in the present study account for about 60·0% of the global records, and around 60·0% of the cases distributed along the southeast coast of mainland China. Teenagers and adults from rural areas are the main groups experiencing infection, and no obvious sex difference was observed.
The primary mode of sparganosis transmission in mainland China during the survey period was via contact (54·6%), with most cases infected through the use of frog flesh as a poultice for self-treatment. This contact transmission was mainly distributed in Southern, Southwestern and Eastern China. This mode of transmission is quite different from other countries. In South Korea and Japan, the main mode was foodborne. Consuming the flesh of snake or fowl has been considered to have nutritional and medicinal effects for ill and weak people in these countries [Reference Cho4]. In Thailand, most patients were infected by drinking raw water contaminated with infected copepods, although there were a few cases caused by application of frog or snake flesh as a poultice [Reference Wiwanitkit15]. Risk factors of mode of transmission in different areas varied in China. For example, the most common risk factor was using frog flesh as a poultice to cure inflammation of the eyes and body surface in Southern and Eastern China [Reference Deng16–Reference Zhou and Lan23]. In Sichuan province, most patients became infected through biting and retaining frog flesh in the mouth as a cure for toothache [Reference Chen24]. There were nine cases in Southern China that had a history of using herbs, i.e. heartleaf Houttuynia herb. This herb grows along water-edges and has detoxification and antipyretic properties in traditional Chinese medicine, and is used as a poultice [Reference Pang18, Reference Li25]. It was speculated that the herbs were contaminated by procercoids or copepods in water. Most cases infected by contact occurred in rural areas before 2000 due to poor medical conditions and local customs.
The second mode of transmission was foodborne, mainly caused by ingesting undercooked meat of the second intermediate host such as frog, snake and other animals [Reference Piao, Jin and Xu26]. There were a few cases infected by special risk factor. For example, most cases (26/34) reported in Henan province were said to be caused by the unusual practice of swallowing live tadpoles to ‘relieve inflammation or internal heat’, and all these cases were confirmed by ELISA [Reference Cui27]. In traditional Chinese medicine, the gallbladder of the snake was believed to have detoxification and antipyretic properties. Ingestion of the gallbladder or drinking bile with wine was a popular practice with people consuming snake. There were six cases infected in this way and one case infected by swallowing the gallbladder of chicken [Reference Ru and Ren28–Reference Zhen31].
The third mode of transmission was waterborne. In rural areas, many farmers were accustomed to routinely drinking untreated water. If the water was contaminated with copepods and/or procercoids, infection might occur.
In 177 cases with no obvious/unknown medical histories, there was one case in a newborn child. Shortly after the child was born, an uplift wound was found at the left ear hairline, from which a plerocercoid of length of 475 mm was removed. It has been established that this disease can also be caused by vertical transmission [Reference Chen32].
Most cases of sparganosis located in the maxillofacial region, eyes and upper limbs, were caused by contact, especially the use of frog flesh as a poultice, accounting for 90·4% (150/166), 90·1% (274/304) and 76·9% (10/13) of cases, respectively. However, for cases of other parts of the body, the first mode of transmission was foodborne followed by waterborne. This implies that there is a close correlation between disease location and mode of transmission.
In past decades great changes have occurred in China regarding the economy, medical and health conditions, popularity of heath knowledge and improved living standards. Customs such as using frog meat as a poultice or swallowing tadpoles for self-treatment were rare in epidemic areas, while the consumption of frogs, snakes, and other wild animals were popular in some areas of China. Therefore, cases caused by contact decreased markedly (from 83·8% pre-1979 to 18·1% post-2000), while foodborne cases increased (from 7·3% to 63·9% in same period), and cases caused by drinking contaminated water also increased. Sparganosis has become one of the important food-/waterborne parasitic diseases in China [Reference Zhou33].
Most cases in the present study were confirmed by post-operative biopsy. Although there were immunodiagnostic and CT/MRI methods for the auxiliary diagnosis [Reference Cui34–Reference Yeo, Yong and Im36], they are not popular in most hospitals in China, especially before 2000. Besides the cases discussed in this study, it is believed that there were more cases not reported due to misdiagnosis or other reasons. Before the 1980s, due to the absence of effective diagnostic methods, there was no report of CNS sparganosis in China. The first domestic case of CNS was reported in 1982 [Reference Zhang37]. After the 1980s, CT/MRI technology was introduced in some hospitals in China, which greatly contributed to surgical therapy for CNS occupied lesions and more sparganosis CNS cases were confirmed by pathological observation or direct observation of parasites post-operatively, but misdiagnosis remained at a high level pre-operatively. In the past decades, CNS sparganosis is the most common of cases reported, accounting for 47·8% of all sparganosis cases [Reference Wang38–Reference Yi, Luo and Liu40].
In conclusion, China is the main epidemic country of sparganosis in the world, the disease is distributed throughout most provinces especially in Southern and Eastern China. The main mode of transmission is via contact, followed by foodborne and waterborne transmission. There are great differences in the main risk factors of sparganosis in different areas due to the customs and eating habits. The tissue/organs involved have a close relationship with the risk factors. The main risk factors have changed over the past decades, from using raw frog flesh as a poultice to consuming frog and snake meat. The tissue/organs involved also changed at the same time, cases of oral/maxillofacial, and eyes decreased and cases of other parts of the body, especially CNS, increased. Now, sparganosis has become one of the neglected but important foodborne/waterborne parasitic diseases in China. In future, not consuming the raw flesh of snakes, frogs, fowl or other animals and not drinking raw water will be the main strategies to prevent sparganosis. Early and effective diagnostic methods and new medications should be developed.
ACKNOWLEDGEMENTS
This work was supported by the National Nature Science Foundation of China (grant no.81260254).
DECLARATION OF INTEREST
None.












