The prevalence of obesity has increased alarmingly over the past several decades. In 2007–2008 the rate among US adults reached 33·8 % overall, up from 22·9 % in 1988–1994 according to the National Health and Nutrition Examination Survey(Reference Flegal, Carroll and Ogden1, Reference Flegal, Carroll and Ogden2). In response, researchers have focused on the environmental context of diet such as food access and availability(3), which can shape dietary habits. The impact of socio-economic factors such as race/ethnicity, income, employment and education on health and weight is well reported(Reference Smith, Cummins and Taylor4–Reference Cummins and Macintyre6). For example, several studies have shown a relationship between lower economic status and poorer diet quality, higher prevalence of food insufficiency and higher obesity rates compared with individuals with higher socio-economic status(Reference Stimpson, Nash and Ju7–Reference Neumark-Sztainer, Story and Hannan10). Consumption of fruits and vegetables is also higher among people with higher socio-economic status and education(Reference Shohaimi, Welch and Bingham11–Reference Irala-Estévez, Groth and Johansson14). This is important, as a diet high in fruits and vegetables has been associated with a decreased risk of chronic diseases such as cancer and coronary artery disease(Reference Stimpson, Nash and Ju7, Reference Shohaimi, Welch and Bingham11, Reference Wallström, Wirfält and Janzon15, Reference Joshipura, Hu and Manson16).
Recently, more attention has focused on the potential impact of an individual's place of residence and whether the components of a healthy diet are readily available and affordable. The term ‘food desert’ was introduced by a resident of public sector housing in the west of Scotland in the early 1990s and first appeared in a 1995 government publication from a policy working group of the Low Income Project Team of the UK Conservative Government's Nutrition Task Force(Reference Cummins and Macintyre6). Since that time, the term ‘food desert’ has been defined in many different ways and no commonly accepted definition currently exists in the literature(Reference Walker, Keane and Burke17). For example, Beaumont et al.(Reference Beaumont, Lang and Leather18) consider a food desert ‘a geographic area where residents experience physical and economic barriers to accessing healthy foods’, whereas Cummins and Macintyre(Reference Cummins and Macintyre6) consider it a ‘poor urban area where residents cannot buy affordable, healthy food’. Together, these definitions reflect important characteristics of a food desert. The US Department of Agriculture (USDA) defines a food desert as an area where the median family income is at or below 80 % of area median family income and at least 33 % of the census tract's population resides more than 1 mile (1·61 km) from a supermarket or large grocery store (for rural census tracts, the distance is more than 10 miles (16·1 km))(19). In recent years, areas of Detroit have been declared food deserts(20, Reference Treuhaft and Karpyn21). Many Detroit residents are low-income individuals without access to reliable public transportation, which can limit access to fresh fruits and vegetables. Smith and Hurst reported that the last large chain of supermarkets, called Farmer Jack, was closed in 2007(Reference Smith and Nathan22). The median household income of residents of Detroit was $US 27 862 v. $US 48 669 for Michigan state residents(23). However, a 2007 report focused on Detroit(20) showed that the Supplemental Nutrition Assistance Program (SNAP; previously known as the USDA Food Stamp Program) was associated with food imbalance in urban Detroit, rather than fast-food consumption as hypothesized. Food imbalance is defined as a the average distance to any mainstream food venue divided by the average distance to a fringe food venue, in contrast to food balance where the distance to mainstream grocers is roughly the same as the distance to the nearest fast-food establishments. The elimination of large, well-stocked grocery stores in Detroit has led to SNAP retailers being primarily so-called ‘fringe’ food locations, such as gas stations, liquor stores, dollar stores, pharmacies and convenience stores. These stores stock largely pre-packaged and canned foods high in sodium, sugar and energy.
In 2007–2008, Gallagher et al. studied the city of Detroit and Metro Detroit area. They examined the distance between the geographic centre of each block and the location of each food venue. Further, they calculated the average distance to any mainstream food venue divided by the average distance to a fringe food venue; data from SNAP were also included in the analysis. Results showed that in Detroit, only 8 % of all SNAP food retailers are small, medium or large grocery stores compared with 92 % fringe locations such as liquor and party stores. Moreover, half the city's population lives in areas where residents have to travel twice as far to reach the closest grocery store compared with the closest fringe food location(20).
Only a few studies have examined the effect of geographic area of residence on dietary intake(Reference Shohaimi, Welch and Bingham11, Reference Diez-Roux, Nieto and Caulfield24, Reference Ellaway and Macintyre25) and findings are inconsistent. There is also a large gap in our knowledge of the effects of residing in a food desert on food shopping patterns, food intake and health outcomes such as obesity(Reference Walker, Keane and Burke17). The goal of the present study was to examine whether area of residence within and outside Detroit, an acknowledged food desert, is associated with food shopping and eating behaviours, dietary intakes and obesity among adults in the Metro Detroit area.
Materials and methods
Study population
In the current cross-sectional study, adult patients were recruited in primary-care clinics: two suburban family medicine clinics, a rural family medicine clinic and two urban community health clinics (pooled as a single site). Data collection took place from August 2009 to February 2010. Approximately 250 adults aged 18 years and older at each site were enrolled. Exclusion criteria included individuals with any of the following conditions: organic brain disease or mental disability that precluded understanding of study participation; <18 years old; non-English speakers who could not read the survey; and those unable to see the survey due to eyesight limitations. After exclusions, 1004 adults were available for participation in the study. The St. John Hospital Institutional Review Board approved the study.
Data collection
The principal investigator or a trained research assistant recruited consecutive participants arriving for scheduled ambulatory visits in the waiting area of primary-care clinics. The survey comprised four sections: demographics; personal health status; a modified diet, transportation and shopping survey(Reference Pearson, Russell and Campbell26); and a subscale from the Diet and Health Knowledge Survey (DHKS)(27). The questionnaire included specific questions about: (i) shopping behaviour, namely type of stores used, frequency and amount of shopping; (ii) number of home-made meals, prepared convenience meals and take-out meals, and number of fruits and vegetables consumed over the last 2 d; and (iii) type of transportation used to get to the store. Participants returning completed surveys were able to enter a raffle for shopping vouchers valued at $US 50 for local grocery stores; funding source for the vouchers was the St. John Hospital Graduate Medical Education Research Committee.
Measurements of main exposure and outcome variables
The main exposure variable, area of residence, was created by categorizing participants according to whether they lived in the city of Detroit or outside the city based on self-reported home zip code. The main outcome variable was BMI (kg/m2). BMI was calculated based on self-reported height and weight and was analysed as a continuous variable. Individuals were also classified as normal weight (18·5 ≥ BMI < 25·0 kg/m2), overweight (25·0 ≥ BMI < 30·0 kg/m2) or obese (BMI ≥ 30·0 kg/m2) using WHO criteria(Reference James, Leach and Kalamara28).
Covariate assessment
Data on additional covariates were collected from the questionnaire, including demographic information (age, gender, site, race, employment status, education, income and SNAP participation), disease status (exercise, smoking, health self-rating, use of supermarkets, farmers’ markets, convenience stores and restaurants) and dietary intakes (servings of home-made foods and prepared convenience foods, fruits, vegetables, snacks and deserts). Transportation and shopping questions were used with permission from Pearson and colleagues(Reference Pearson, Russell and Campbell26) and were modified slightly for our study population. Use of supermarkets refers to large markets in the Detroit area such as Krogers or Meijers. Markets refer to smaller markets and local farmers’ markets such as Eastern Market. Convenience stores refer to stores like 7-Eleven, gas stations and drug stores. The DHKS was originally a telephone follow-up survey to the Continuing Survey of Food Intakes by Individuals conducted by the USDA as part of the National Monitoring and Related Research Program(Reference Obayashi, Bianchi and Song29). We used the twelve-question subscale from the DHKS called ‘Perceived value of healthy eating’(27). This short-form version was developed based on the original 149-item 1994–1996 DHKS and has been shown to be reliable and valid(Reference Obayashi, Bianchi and Song29).
Statistical analyses
Sample characteristics were described using means and standard deviations for continuous variables (BMI, age, servings of home-made foods and prepared convenience foods, fruits, vegetables, snacks and deserts) and frequencies (number and percentage) for categorical variables (gender, site, race, employment status, education, income, SNAP participation, exercise, smoking, health status self-rating, obesity, hypertension, diabetes mellitus, anaemia, kidney disease, use of supermarkets, farmers’ markets, convenience stores and restaurants). Bivariate associations between eating and shopping behaviours and area of residence were examined using the χ 2 test for categorical variables and Student's t test for continuous variables. We evaluated whether the association between each independent categorical covariate and BMI was significantly different for people living within and outside Detroit through individual ANOVA models that included an interaction term between area of residence and the covariate (e.g. Detroit × gender); for each continuous covariate, we evaluated the association between the covariate and BMI with Spearman's correlation coefficient (ρ).
Our main analyses employed multivariable linear regression models to examine associations between our main exposure variable, area of residence (living in Detroit v. outside Detroit), and BMI. We treated our outcome as a continuous variable due to the high prevalence of obesity in the sample (74 %) and to maximize statistical power; living outside Detroit was the referent. In our analysis, we examined the effect of each of the covariates on the relationship between living in a food desert and BMI. Due to the large amount of variables, we first grouped our variables into the categories of demographics (age, sex, employment status, income, education, having access to a car and SNAP participation), health-related (exercise, smoking, health self-rating and presence of disease: hypertension, diabetes mellitus, anaemia or kidney disease) and grocery shopping (use of supermarkets, markets, convenience stores and restaurants). We then built the model progressively. Model 1 was a simple model including only area of residence. Model 2 was adjusted for race/ethnicity. Model 3 was adjusted for additional demographic variables (age, sex, employment status, income, education, having access to a car and SNAP participation). Model 4 built on Model 3 and further adjusted for exercise, smoking, health self-rating, presence of disease (hypertension, diabetes mellitus, anaemia or kidney disease) and SNAP participation. The final, fully adjusted model (Model 5) included all previous covariates along with shopping behaviours (use of supermarkets, markets, convenience stores and restaurants), dietary intakes (servings of home-made foods and prepared convenience foods, fruits, vegetables, snacks, desserts) and diet knowledge. We quantified the measures of association between each covariate and BMI in a single, fully adjusted multivariable linear regression model (Model 5). Secondary to our concerns regarding the relationship between race/ethnicity distribution and area of residence, we checked for collinearity between these variables. We used the cut-offs for tolerance (>0·10) and variance inflation factors (<5·0); there were no violations. In secondary analyses based on observed results we examined the effect of SNAP participation on BMI among Detroit residents only.
Analyses were performed using the statistical software packages SAS version 9·1 and SPSS for Windows version 12·0; P values less than 0·05 were considered statistically significant. Our conceptual model showing the association between area of residence and obesity that guided our analysis is shown in Fig. 1.

Fig. 1 Hypothesized conceptual model illustrating the associations between living in a food desert such as Detroit and obesity among adults
Results
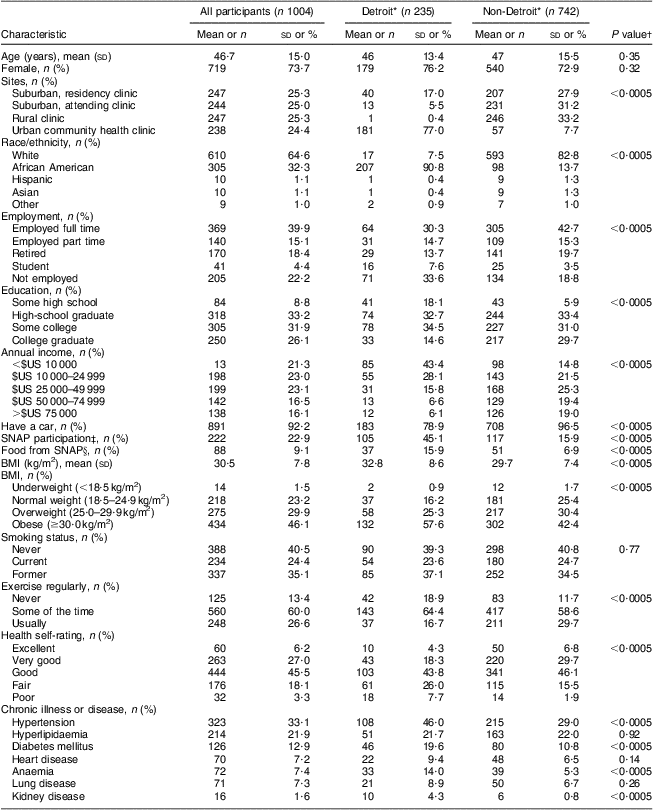
The mean age of adult participants (n 1004) was 46·7 (sd 15·0) years (range 18–93 years), with males comprising 26 % of the sample (n 257; Table 1). Thirty-three per cent were high-school graduates, 32 % had at least some college and 26 % were college graduates. Participants were mainly Caucasian (65 %), followed by African American (32 %). Forty-four per cent lived with an income that is estimated at poverty level and 55 % worked full or part time. About 30 % were overweight and 46 % were obese. Hypertension (33 %), hyperlipidaemia (22 %) and diabetes mellitus (13 %) were the most frequently self-reported health conditions. Approximately 25 % were current smokers. We detected significant differences between Detroit participants v. those living outside Detroit in race/ethnicity (P < 0·0005), employment (P < 0·0005), education (P < 0·0005), income (P < 0·0005), SNAP participation (P < 0·0005), BMI (P < 0·0005), exercise (P < 0·0005) and presence of a chronic disease or illness such as hypertension (P < 0·0005), diabetes mellitus (P = 0·0005), anaemia (P < 0·0005) and kidney disease (P < 0·0005).
Table 1 Characteristics of the entire sample and stratified by area of residence: adults (n 1004) from Metro Detroit, MI, USA, August 2009–February 2010

SNAP, Supplemental Nutrition Assistance Program.
*Detroit v. non-Detroit variable was defined based on self-reported zip code.
†Compared by Student's t test (continuous variables) or the χ 2 test (categorical variables).
‡SNAP participation refers to WIC (Special Supplemental Nutrition Program for Women, Infants, and Children) or Bridge Card.
§Food from SNAP refers to programmes such as Gleaners, Capuchins, or a church group.
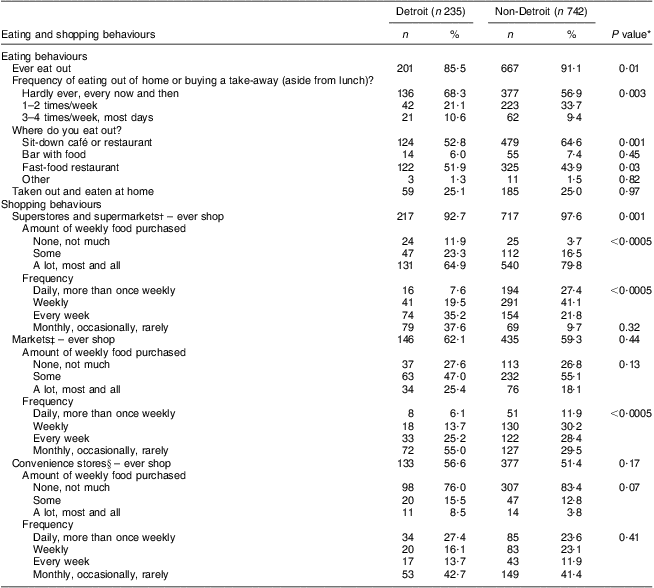
A slightly higher proportion of participants living outside Detroit reported ever using supermarkets (98 % v. 93 %, P = 0·001), more frequent use of supermarkets (P < 0·0005), using supermarkets for larger weekly food purchases (P < 0·0005) and using fresh markets more often (P < 0·0005), compared with those living in Detroit (Table 2). A smaller proportion of those living in v. outside Detroit ate out (hardly ever: 68 % v. 57 %; 1–2 times/week: 21 % v. 34 %; most days: 11 % v. 9 %, P = 0·003); a lower percentage ate out at places like sit-down cafés (P = 0·001) while a higher proportion ate at fast-food restaurants (P = 0·03). A higher BMI was observed among participants living in v. outside Detroit among those who shopped at superstores (32·9 (sd 8·6) v. 29·6 (sd 7·4) kg/m2, P < 0·0005), markets (32·8 (sd 8·6) v. 29·6 (sd 7·4) kg/m2, P < 0·0005) and convenience stores (33·0 (sd 9·4) v. 29·80 (sd 8·0) kg/m2, P = 0·001; data not shown). Bivariate associations between BMI and dietary intakes and food behaviours among participants living within and outside Detroit are presented in Table 3.
Table 2 Bivariate associations between eating and shopping behaviours according to area of residence among adults (n 1004) from Metro Detroit, MI, USA, August 2009–February 2010

*Evaluated with the χ 2 test.
†Supermarkets refer to large markets in the Detroit area such as Krogers or Meijers.
‡Markets refer to smaller markets and local farmers’ markets such as Eastern Market.
§Convenience stores refer to stores such as 7-Eleven, party stores, gas stations or drug stores.
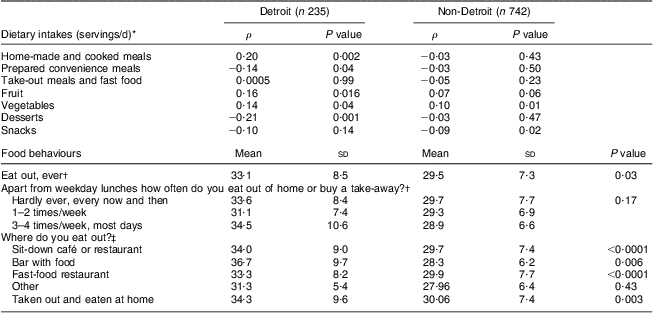
Table 3 Bivariate associations between BMI and dietary intakes and food behaviours according to area of residence among adults (n 1004) from Metro Detroit, MI, USA, August 2009–February 2010

*Associations between BMI and food intakes (servings/d) among participants living within and outside Detroit were measured using Spearman correlation coefficients (ρ).
†Associations between food behaviours and BMI of participants living within Detroit and outside Detroit were measured using ANOVA.
‡Associations between food behaviours and BMI of participants living within Detroit and outside Detroit were measured using a t test.
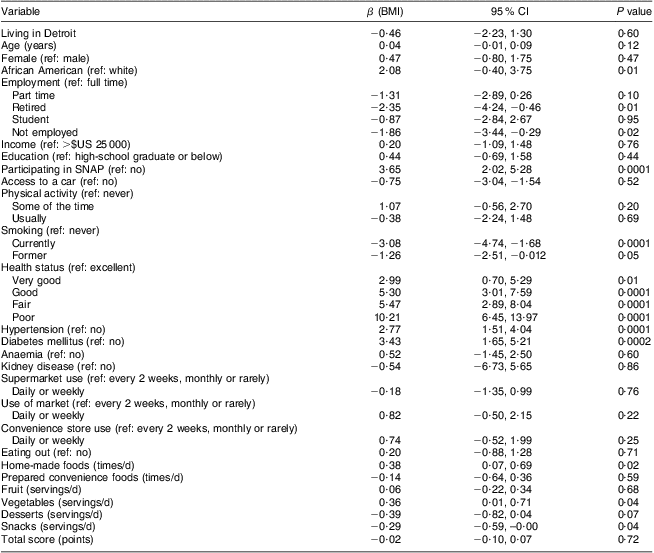
In unadjusted linear regression analyses, participants living in Detroit had a 3·06 (95 % CI 1·91, 4·21) kg/m2 larger BMI than those living outside Detroit (P < 0·0001; Table 4). However, the effect was attenuated when adjusted for potential confounders such as demographics, disease status, shopping and food behaviours, dietary intakes and diet knowledge (β = −0·46 kg/m2, 95 % CI −2·23, 1·30 kg/m2, P = 0·60). In fully adjusted multivariable models (Table 5), significant associations with BMI included: SNAP participation (β = 3·65 kg/m2, 95 % CI 2·02, 5·28 kg/m2, P = 0·0001); self-reported health status (very good v. excellent: β = 2·99 kg/m2, 95 % CI 0·70, 5·29 kg/m2, P = 0·01 | good v. excellent: β = 5·30 kg/m2, 95 % CI 3·00, 7·59 kg/m2, P < 0·0001 | fair v. excellent: β = 5·47 kg/m2, 95 % CI 2·89, 8·04 kg/m2, P < 0·0001 | poor v. excellent: β = 10·21 kg/m2, 95 % CI 6·45, 13·97 kg/m2, P < 0·0001); having a diagnosis of hypertension (β = 2·77 kg/m2, 95 % CI 1·51, 4·04 kg/m2, P < 0·0001); having a diagnosis of diabetes mellitus (β = 3·43 kg/m2, 95 % CI 1·65, 5·21 kg/m2, P = 0·0002); and smoking status (current v. never: β = −3·08 kg/m2, 95 % CI −4·48, −1·68 kg/m2, P < 0·0001 | former v. never: β = −1·25 kg/m2, 95 % CI −2·51, −0·01 kg/m2, P = 0·05). In secondary analysis among Detroit participants only, there were no differences in BMI comparing SNAP participants v. non-participants (32·9 (sd 8·5) v. 32·9 (sd 9·9) kg/m2, P = 0·98; data not shown).
Table 4 Linear regression analyses showing the unadjusted and multivariable-adjusted associations between living in a food desert and BMI among adults (n 1004) from Metro Detroit, MI, USA, August 2009–February 2010

SNAP, Supplemental Nutrition Assistance Program.
*Demographic variables included age, sex, race, employment, income, education and having access to a car.
†Health behaviours and disease status variables included physical activity, smoking, health self-rating, hypertension, diabetes mellitus, anaemia and kidney disease.
‡Shopping and eating behaviour variables included use of supermarkets, markets and convenience stores, and eating out.
§Dietary intake variables included servings of home-made foods, prepared convenience foods, fruit, vegetables, snacks and desserts.
∥Diet knowledge is the total score of twelve questions from the Diet and Health Knowledge Survey.
Table 5 Linear regression analysis showing multivariate-adjusted associations between individual covariates and BMI* among adults (n 1004) from Metro Detroit, MI, USA, August 2009–February 2010

ref, referent category; SNAP, Supplemental Nutrition Assistance Program.
*All variables were included in one multivariable adjusted model (Model 5).
Discussion
The current cross-sectional study evaluated the effect of living in Detroit, a food desert, on food shopping and eating behaviours, dietary intakes and BMI. Obesity is a major problem throughout the Detroit area and the prevalence (57·6 %) greatly exceeds recent estimates for the USA (33·8 %) made by the Centers for Disease Control and Prevention(Reference Flegal, Carroll and Ogden1). While strongly associated with BMI in unadjusted analysis, the effect of living in Detroit was greatly attenuated once adjusted for confounders such as demographics, disease status, shopping patterns, dietary intakes and diet knowledge. These results suggest that these variables confound and/or mediate the effect of living in a food desert on obesity. Our study thus underscores the importance of considering the multifaceted and complex nature of the overall food environment when examining the impact of food deserts on health outcomes. To the best of our knowledge, ours is the first study among adults that has examined the impact of living in a food desert on BMI while considering a wide range of potential covariates and therefore makes an important contribution to the literature.
Previous studies have shown conflicting evidence regarding the effect of area of residence on dietary intakes. Our results agree with those of An and Strum(Reference An and Strum30, Reference Shier, An and Strum31) who found no evidence to support the hypothesis that easier access to supermarkets improves dietary intakes and reduces BMI. However, previously, Diez-Roux et al. (Reference Diez-Roux, Nieto and Caulfield24) and Ellaway and Macintyre(Reference Ellaway and Macintyre25) observed a decrease in fruit and vegetable consumption in residential deprivation areas. In contrast, Pearson et al. (Reference Pearson, Russell and Campbell26) found that fruit and vegetable prices and socio-economic deprivation did not influence fruit or vegetable consumption, although sociocultural attitudes toward foods were a crucial element. Kwate(Reference Kwate32) further argues that race-based residential segregation is a fundamental cause of fast-food density in African American neighbourhoods. Specifically, he described how segregation tends to create localized geographic areas targeted by fast-food restaurant corporations, fostering economics, business conditioning and land use. These characteristics increase the likelihood of fast-food proliferation. Additionally, McDermott and Stephens showed that diets rich in foods from convenience stores are more expensive than a well-planned menu from budget foods available at large supermarkets(Reference McDermott and Stephens33). Cultural and ethnic background, economy and infrastructure thus play key roles in influencing eating habits and provide additional targets whereby health and disease risk may be modified.
Our results indicate that age, income and employment have modest effects on the association between residence area and BMI when compared with disease status and receiving food stamps. Participants living in Detroit had a higher BMI (32·8 (sd 8·6) kg/m2) compared with people living outside Detroit (29·7 (sd 7·4) kg/m2, P < 0·0001), but the effect was attenuated when adjusted for demographics, disease status, shopping patterns, food intake and diet knowledge (β = −0·46 kg/m2, 95 % CI −2·23, 1·30 kg/m2, P = 0·60), as noted. Our multivariable linear regression model showed that our set of covariates explained 25 % of overweight/obesity. Further, analysis of BMI for Detroit residents v. non-residents in relation to shopping behaviours revealed no differences (data not shown). Rather, simple demographics played a crucial role in these associations, such as race/ethnicity, employment status, access to a car and participation in SNAP. Living in the ‘motor city’, Detroit residents drive almost everywhere. The role of transportation in Detroit is very specific and it could alter the definition of the food desert and shopping environment, as recently pointed out by An and Strum(Reference An and Strum30, Reference Shier, An and Strum31). Future research could help answer this question by considering together areas in which people work as well as where they live, which we did not do in the present study. We also did not evaluate whether participants had skills and/or time to plan for food shopping and preparation, which was shown to be important in another study(Reference McDermott and Stephens33). These and other factors could account for other additional variation in BMI not explained by our model when comparing those within and outside Detroit.
We observed a strong correlation between living in Detroit and race/ethnicity in our study (r = 0·70), which is concordant with US Census statistics: the population of Detroit is 91 % African American (US Census: 82·7 % African American), 8 % White (US Census: 10·6 %) and 0·4 % Asian (US Census: 1·1 % Asian)(23). Because living in Detroit was so highly correlated with race/ethnicity in our study, distinguishing independent associations between residence area, race/ethnicity and BMI was not possible. While our tests for confluence were not violated using pre-specified cut offs for tolerance and variance inflation factors, future studies should examine the association between food deserts and obesity using a population of greater diversity to shed further light on the relationship of race/ethnicity to food deserts and obesity.
Our study has several limitations. First, it had a cross-sectional design. As such, the exposures and outcomes were assessed at the same point in time such that the temporal relationship cannot be established. It is possible that residents with higher body weight may choose to live in or transfer to an area with an unhealthier food environment, and our design did not allow us to investigate this possibility. Our sample was not randomly selected and is not representative of the US population or of individuals living in food deserts as a whole. Furthermore, our sample was recruited from clinical primary-care sites, so participants who agreed to participate may have been more health conscious compared with those who declined to participate or who do not seek regular care at such clinics. Additionally, men often avoid preventive health care, which may have contributed to the majority of our sample being women; this translated into a higher obesity prevalence than the US average(Reference Flegal, Carroll and Ogden1, Reference Flegal, Carroll and Ogden2). We tried to enrol consecutive patients to minimize selection bias. In addition, the participants’ self-reported height and weight may result in measurement error, although previous studies have shown that self-report is a valid measure of BMI in epidemiological studies(Reference Gorber, Tremblay and Moher34, Reference Kuczmarski, Kuczmarski and Najjar35). Similarly, participants self-reported their food intake for only 2 d, which may not reflect usual intake due to within-person variation. That said, the direction of the associations between BMI and food intakes, including consumption of vegetables (positive association), prepared convenience foods (negative association), desserts (negative association) and snacks (negative association), was in the opposite direction to that expected, suggesting reverse causality. In other words, participants with higher BMI perhaps changed their diet in response to their weight to consume more vegetables and fewer prepared convenience foods, desserts and snacks. As well, although the food desert area was defined based on self-reported zip code, Detroit has been previously defined as a food desert(20, Reference Treuhaft and Karpyn21) and we do not have reason to believe that participants had problems recalling zip codes. To assess the validity of whether zip code data were accurately reported, we examined concordance between where participants completed the survey and where they reported living. We found that most participants who were recruited in Detroit free clinics accurately reported the zip codes as a resident for city of Detroit. Specifically, we found 99 % concordance for the rural family medicine clinic, 95 % for the Masonic suburban family medicine clinic, 84 % for the suburban family medicine clinic, and 76 % for the urban community health clinics (data not shown). Defining exposure based on the 5-digit zip code rather than the zip+4 or street address may not have been detailed enough to show the effect of residence area. Future studies might consider using more sophisticated technologies such as GPS (global positioning systems) from participants’ smart phones to better elucidate area of residence effects on obesity, as well as area of work effects. Finally, a more detailed account of store inventories to better understand differences between various stores where participants shopped would be helpful. Unfortunately, this kind of research is very expensive and difficult to undertake in large epidemiological studies(Reference An and Strum30).
Conclusion
Overweight and obesity are major public health problems throughout the Detroit area. However, living in Detroit, a recognized food desert, was not associated with BMI once potential covariates were considered. These findings suggest that the relationship between obesity and area of residence is not explained simply by access to supermarkets but is influenced by other aspects such as sociodemographic factors and health status, which may confound or mediate the association. Additional research is needed to further disentangle the complex associations between living in a food desert and obesity. Such research will be beneficial in informing public-health professionals, policy makers and primary-care physicians where to direct obesity prevention and treatment strategies.
Acknowledgements
Sources of funding: K.B. is the recipient of the Physician Training Award in Preventive Medicine, American Cancer Society (PTAPM # 97-185-12). The Graduate Medical Education Department of St. John Hospital and Medical Center, Detroit, MI provided funding for the study. The funding agencies played no role in the design or conduct of the study; the collection, management, analysis or interpretation of the data; or the preparation, review or approval of the manuscript. Conflicts of interest: None of the authors had any conflicts of interest to disclose. Authors’ contributions: K.B., P.W., R.T.S.-M. and D.L. designed the research project; D.L. and P.W. collected the data; P.K.N. and K.B. designed the study questions; K.B., R.T.S.-M., and M.W. analysed the data; K.B., P.W., R.T.S.-M., D.L., M.W. and P.K.N. interpreted the data; K.B. and P.K.N. wrote the manuscript and have primary responsibility for the final content. All authors read and approved the final manuscript. Acknowledgements: The authors are grateful to MetroNet, a research group in Wayne State University, which helped recruit participants into the study.