INTRODUCTION
Helicobacter pylori, a bacterium affecting the stomach and intestinal tract, infects approximately half of the world's population and causes duodenal and gastric ulcers [Reference Brown1]. H. pylori is a Class I carcinogen. Chronic inflammation, associated with long-term symptomatic infection, results in gastric adenocarcinoma in about 2% of infected persons [Reference Peek and Blaser2, Reference Go3]. Gastric cancer mortality rates in American Indians/Alaska Natives are 1·5 times higher than the general US population, indicating an elevated prevalence of H. pylori infection [Reference Wiggins4–7].
H. pylori seropositivity indicates active or past infection, and persists for months to years after spontaneous or therapeutic resolution of active infection. Large-scale studies demonstrate that the seroprevalence of H. pylori in the US adult population aged ⩾20 years is 32% [Reference Everhart8, Reference Simon, Hudes and Perez-Perez9]. In US adolescents and children aged <20 years, seroprevalence of H. pylori is 25% [Reference Staat10]. A study of Alaska Natives reported a 75% seroprevalence [Reference Parkinson11].
Specific knowledge is limited regarding active H. pylori prevalence in American Indian/Alaska Native populations in the lower 48 states. Active infection is determined by the urea breath test (UBT), in which the subject ingests a dose of carbon isotope-labelled urea. Increased labelled CO2 production, catalysed by urease enzymes of the infecting organisms, is detected and proportionately measured in a stored breath sample [Reference Graham12–Reference Graham14].
Although its route of transmission and specific prevention methods are unknown, research indicates that H. pylori is transmitted by the faecal–oral route or by the oral–oral route through vomitus or saliva [Reference Parsonnet, Shmuely and Haggerty15]. Previous studies identified household crowding, lower socioeconomic status (SES), and contaminated drinking water as risk factors for infection [Reference Brown1, Reference McKeown16, Reference Nurgalieva17].
In October 2005, Indian Health Service (IHS) epidemiologists were invited to investigate a perceived increase in H. pylori cases in a Northern Plains American Indian reservation. Local residents were concerned that transmission of H. pylori might be occurring through the drinking-water supply. Medical chart and clinical laboratory test result reviews revealed that cases of H. pylori had increased during the previous 3 years. The investigation began in November 2005, with the goals of determining the prevalence of active H. pylori infection and identifying risk factors for infection. We report the results of the investigation and describe the methods used to address the challenges of survey sampling in a rural population.
METHODS
This investigation underwent human subjects review at the U.S. Centers for Disease Control and Prevention and was determined to be public health practice, not research.
Study design and sampling
We conducted a cross-sectional survey, with participants selected by two-stage simple random sampling. We determined that a pre-existing geocoded emergency medical system (EMS) database of all buildings within the reservation offered a suitable sampling frame. The database included records of buildings identified by global positioning system (GPS) coordinate pairs (latitude and longitude) [18, 19]. Thus, we were able to program these coordinates into GPS receiver units to navigate directly to the sampled buildings. We were informed that one neighbourhood of 15 houses did not have coordinates in the database. We included placeholders in the sampling frame for this group. As soon as coordinates were obtained, the five randomly selected houses from the 15 were included in recruitment efforts. Because all houses were included, the EMS database offered a complete universe of the study population in households.
Our goal was to recruit a sample size of 316 participants to estimate the population prevalence of H. pylori. In the first sampling stage, 1580 records in the database were assigned random numbers and then sorted from lowest to highest number. The first 316 records from the list were selected to recruit participants. To address concerns that severe winter weather might limit areas of travel and prevent complete data collection, we divided the sample into four waves of 79 houses each. Using maps created for each wave, the overall distribution of geocoded sampled vs. unsampled buildings were visually examined to ensure that all areas of the reservation were represented. Each wave included locations randomly distributed throughout central towns and remote ranches and farms to ensure that the participants and their drinking-water sources would be representative. Recruitment was completed in each wave before moving on to the next. If no one was at home during an initial visit, the home was visited at least twice more. Commercial buildings were excluded upon discovery by field teams and duplicate GPS coordinate entries were deleted. The four waves of household recruitment and interviews began in November 2005 and ended in January 2006. Household sampling and navigation maps were created using Arcview Version 3.2a software (ESRI, USA).
Participant eligibility
In the second sampling stage, we randomly selected one person from all eligible household members. Given limited resources, we chose to compare households and could not afford sufficient testing to explore potential intra-household transmission dynamics. The UBT is difficult to administer to children aged <5 years. In addition, certain medications interfere with the test results. The following inclusion criteria were applied: minimum age of 5 years; no report of treatment with a proton pump inhibitor, bismuth subsalicylate, or an antimicrobial within the 2 weeks prior to interview; and no report of treatment for H. pylori within the previous 4 weeks. Length of residency was not an inclusion criterion; however, all participants had lived on the reservation for at least 1 year. Adult participants and parents of minor participants gave written informed consent and minors gave assent.
Questionnaire
Trained interviewers administered a standard questionnaire regarding medication use; symptoms of abdominal pain; family history of stomach cancer or ulcer; personal history of alcohol or tobacco use; household characteristics (past and current places of residence, number of rooms in current home, number of household members, highest paternal education level by school grade); and living conditions such as type of drinking water used and home tap-water source.
Urea breath tests
UBT status (positive vs. negative) was the main outcome measure. We used the BreathTek™ UBT (Meretek Diagnostics, USA), described elsewhere [Reference Graham12–Reference Graham14], to qualitatively detect cases of active H. pylori infection. Participants were asked to refrain from eating, drinking, or smoking for 1 h before taking the UBT. Each participant was instructed to give a baseline breath sample directly into a test bag before drinking a 75-ml non-radioactive 13C-labelled urea powder dissolved in a distilled water solution. One additional breath test was collected 15 min later. The pre- and post-test breath samples were analysed by gas/isotope ratio mass spectrometry (UBiT®-IR300, Meretek Diagnostics) to measure the derived 13CO2. We defined a positive test for active H. pylori infection as an increase in the 13C/12C isotope ratio of 6/1000 over the baseline breath sample, as recommended by Graham & Klein [Reference Graham and Klein13]. UBiT®-IR300 has 95% sensitivity and specificity for diagnosis of active infection. More information is available on the Quest Diagnostics website [20].
Statistical analysis
To account for the two-stage simple random sampling design, we used relevant weights to adjust for unequal selection probabilities for each participant. Weights were constructed for the first-stage probability of the household being selected from the EMS database and the second-stage probability of the participant being selected from all eligible persons in the household. Person weights were calculated as
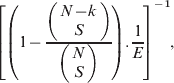 $$\left[ {\left( {1 \minus {{\left( {\matrix{{N \minus k} \cr S \cr} } \right)} \over {\left( {\matrix{ N \cr S \cr} } \right)}}} \right).{1 \over E}} \right]^{ \minus \setnum{1}} \comma $$
$$\left[ {\left( {1 \minus {{\left( {\matrix{{N \minus k} \cr S \cr} } \right)} \over {\left( {\matrix{ N \cr S \cr} } \right)}}} \right).{1 \over E}} \right]^{ \minus \setnum{1}} \comma $$where N is the number of buildings in the EMS database, S is the sample size and E is the number of eligible persons in a household. The term, k, accounts for the number of times a pair of GPS coordinates occurred in the EMS database [Reference Levy and Lemeshow21]. We examined both unweighted and weighted descriptive statistics for UBT status using prevalences; and for the risk factors for active H. pylori infection, mean values and proportions (Table 1).
Table 1. Prevalence and risk factors – active Helicobacter pylori infection in an American Indian Population, 2005–2006

CI, Confidence interval.
The demographic characteristics and survey responses of subjects with a positive UBT were compared to those of subjects with a negative UBT using person weights and univariable logistic regression for each risk factor (Table 2). Next, we conducted a multivariable logistic regression to identify and better understand the relationship between risk factors for a positive UBT. Because of the large number of risk factors considered, we used a forward selection strategy for logistic regression model building. Variables were considered for inclusion in the model based on their potential as risk factors for a positive UBT or for their potential as confounders. Variables were entered into the model in order of the strength of their univariable association with UBT status. Regression models were assessed via the likelihood ratio χ2 statistic test. An α-level of 0·1 was used to determine which variables were retained during model building. All interaction terms that were interpretable and biologically plausible were considered and evaluated using the same inclusion criteria for risk factors and confounders.
Table 2. Active Helicobacter pylori infection and associated risk factors in an American Indian population, 2005–2006

OR, Odds ratio; CI, confidence interval.
* Final regression model: log odds(positive urea breath test) = −2·44 + 0·46(age) – 0·10(age*ln(age)) + 1·34(number in household) – 0·14(number in household)2 – 0·42(number of rooms in home) + 1·21(public water supply as primary drinking water) + 0·38(current smoker).
Five risk factors were modelled as continuous variables. Demographic variables included age in years, and paternal education level as an indicator of SES status. Because children as young as 5 years were eligible for this investigation, the participants' own education level was not a uniform reflection of lifetime educational attainment across the entire sample. We looked at three continuous measures of household crowding: household size defined as the number of people living in the house, the number of rooms in the current home, and the number of people per room taken as the ratio of household size divided by the number of rooms in the house. Scale identification of continuous variables was achieved using statistical tests and graphs from SAS® proc gam (Generalized Additive Models). Statistical analysis was performed using SAS® version 9.3 (SAS Institute Inc., USA) and Stata® version 8 (StataCorp, USA).
RESULTS
Recruitment
Twenty (6%) of the 316 sampled buildings were duplicate entries and were excluded. We located all of the remaining 296 buildings through GPS navigation; however, 17 (6%) commercial buildings were excluded. Of the 279 residences, 35 (13%) were vacant at the time of the visit. Of the 244 occupied households, 228 (93%) had at least one eligible person. Of these, 61 (27%) refused to participate or had incomplete recruitment. A total of 167 (73%) persons were interviewed. One participant who did not complete a scheduled UBT was excluded, leaving 166 participants for statistical analysis. Relative to the 2000 Census total population, this sample represents about 5–6% of the persons living on the reservation.
Descriptive statistics
In general, when sampling weights were taken into account, the distribution of the outcome and risk factors of interest were similar to those of the unweighted estimates. One minor difference was noted between unweighted and weighted proportions of males to females (Table 1).
In the following, we refer only to weighted estimates. Active H. pylori infection was detected in 55·0% of the participants. A history of previous H. pylori diagnosis was reported by 8·0%, of whom 27·5% had a positive UBT at the time of this investigation. Of those with no previous diagnosis of H. pylori, 57·2% had a positive UBT. Forty-one per cent of the participants reported having a family history of stomach cancer or ulcers.
A total of 54·8% of the participants lived in the reservation's most densely populated area. The mean age of participants was 31·4 years (range 5–88 years), while 52·0% of adults aged ⩾18 years were employed at least part time during the last 12 months. Mean household size was 4·6 persons (range 1–10). Although 43·6% reported currently living in homes served by a public water supply, only 8·8% of the participants reported using it as their primary home drinking-water source. Mean paternal education level was 2·8 years. In the USA this is equivalent to the participant's father having attended school until 8 or 9 years of age and having <3 years of formal education. A total of 31 participants did not know or refused to report paternal education, thereby limiting its utility in this population.
Weighted regression analyses
Table 2 shows the results of the logistic regression using person weights. Univariable odds ratios (ORs) are presented for the variables considered for the multivariable model. Of the three measures of household crowding, household size and the number of rooms in the house were retained, but not the number of people per room. Based on the forward selection criteria (α = 0·10), current smoking status remained in the multivariable model. It was also retained as a confounder of the relationship between age and UBT status. Smoking cigarettes was found to increase the odds of a positive UBT; however, the statistical significance of the result was marginal. Factors significantly associated with active H. pylori infection included age, household size, the number of rooms in the house, and having a public water supply as the primary drinking-water source at home.
Two continuous variables, age and household size, were nonlinear predictors of the log-odds of a positive vs. a negative UBT (Table 2). In both cases, quadratic and near quadratic functions gave the best fit in logistic regression models. The partial prediction plots in Figure 1 (along with associated statistical tests using SAS® proc gam) reflect this relationship to UBT status (P = 0·017 and P = 0·004, respectively). The non-parametric effect of number of rooms in the house, although revealing a quadratic pattern, was not statistically significant (P = 0·307).

Fig. 1 [colour online]. The relationship between urea breath test status with age and with factors for household crowding in an American Indian population, 2005–2006. 95% Confidence intervals are shown.
The odds of a positive UBT was found to increase up to age 43·6 years, after which it decreased. In such a relationship, the magnitude and significance of the OR depends on the age used as the referent and that used for comparison. For example, an increase from age 30–40 years results in an OR of 1·71 [95% confidence interval (CI) 1·0–2·8]. A similar nonlinear relationship holds for household size, where the maximum odds of a positive UBT was observed for a household size of 4·8 persons, after which it decreased with additional household members. As an example, an increase in household size from the first quartile (n = 2) to the third quartile (n = 5) results in an OR of 5·9 (95% CI 1·6–21·8). The number of rooms in the house was inversely and linearly related to the odds of a positive UBT. As the number of rooms in the house increased, the odds of UBT decreased (OR 0·66, 95% CI 0·47–0·92) (Table 2).
The strongest association observed for increased odds of a positive UBT was for those whose primary source of drinking water was obtained from a public water supply. Controlling for other factors in the model, the OR was 11·2 (95% CI 2·6–48·8).
No interactions were identified between any of the variables in the model, including the interaction between household size and the number of rooms.
DISCUSSION
The GPS, a US Government-owned utility [18, 19], allowed us to use a convenient geocoded sampling method and GPS navigation units to overcome the challenge of locating randomly selected homes in a rural community. This sampling method made a potentially difficult and time-consuming task simple and efficient. We were able to locate even the most remote households with ease. By using a pre-existing EMS database accurately geocoded for every building in the study area, we sampled from a complete universe of households.
This is the first report of the epidemiology of active H. pylori infection within an American Indian community outside Alaska. The overall prevalence of active H. pylori infection in this community was 55·0%. The prevalence of positive UBT was 79·5% in persons aged 30–39 years. This prevalence is higher than the seropositivity estimated in the general US population during the late 1990s [Reference Everhart8–Reference Staat10]. In comparison, active infection in the general population should be even lower because seropositivity persists for months to years after spontaneous or therapeutic resolution of infection. Some Alaska Native communities have reportedly higher prevalences of active H. pylori infection (81%, unpublished data, H. pylori Village Impact Survey, CDC/Arctic Investigation Program, 1996) compared to other published results for Alaska Natives [Reference Parkinson11] and compared to our own observations in this American Indian population. Future studies should assess both seropositivity and the incidence or prevalence of active H. pylori infection to aid comparability in different studies and populations.
Our finding of a marginal association between cigarette smoking and active H. pylori infection is similar to other reports in the literature, despite differences in the methods and populations studied [Reference Bateson22, Reference Fontham23]. Our investigation included children and adolescents; therefore, the likelihood of current smoking would be very different in this age group compared to adults in this population and with other studies of adults. Both H. pylori infection and smoking are related to higher risk of intestinal metaplasia [Reference Peleteiro24]; thus, our observation of a suggested relationship is not unexpected. Since infection and smoking have been observed to contribute to gastric cancer, both jointly and independently in prospective studies [Reference Shitaka25], additional studies of such modifiable risk factors, and detection and treatment for different virulence subtypes, are important to establish public health intervention strategies.
The association we identified between drinking water and active H. pylori infection lends intriguing evidence to the theory that water contaminated by sewage is a potential route of H. pylori transmission. At least one study has reported an association between H. pylori seropositivity and consumption of untreated surface water [Reference Nurgalieva17]. Ours is the first study to document an association between exposure to drinking water from a publicly treated source and active H. pylori infection. Our investigation did not examine the quality of the public water system. At the time of the investigation, reliable laboratory techniques did not exist to demonstrate the presence of living and infectious H. pylori bacteria in the water.
The perception of a causal association with the public water supply probably influenced the majority of participants (91·2%) to consume drinking water from other sources. It is unknown whether this choice was a source of bias in this investigation. Since the time of this investigation, a new water supply and treatment facility has been constructed. New surface water intakes have been moved away from a neighbouring system's discharge. Water quality issues continue to be evaluated, and to date, the public water supply has neither been implicated nor exonerated as a possible causal factor in the incidence of active H. pylori infection (Barbara Burkland, U.S. Environmental Protection Agency, personal communication).
Our finding that the likelihood of active H. pylori infection increased as the number of rooms in the homes of tribal residents decreased is consistent with reports of crowding as a significant risk factor. The number of rooms in the current home might be a proxy measure for another SES factor, such as current household income, which was not assessed in this investigation. The importance of household crowding is further supported by the finding of increased H. pylori infection as the number of people in the household increased to about five persons. The relatively small number of households with more than five members and the associated increase in variability that results, might explain the nonlinear shape of this relationship.
Our findings are subject to certain limitations. The cross-sectional survey design in our investigation limits our ability to assess a causal association between exposure and disease. These findings are not likely to be generalizable to other populations, as the community has unique environmental and cultural characteristics such as cold winters, a relatively large and central town area with a public water supply, and indoor winter gatherings. The large number of participants who did not know or report paternal education level indicates a need to create more culturally relevant SES measures. Exclusion of persons taking antimicrobials or proton pump inhibitors might have resulted in underestimation of disease prevalence because older adults tend to use proton pump inhibitors more frequently. We might have systematically under-enrolled members of this age group, potentially resulting in the lower prevalence of infection observed among them. Sampling challenges existed with the pre-existing EMS database, including duplicate locations and inclusion of public or commercial buildings. Nevertheless, we were able to account for this with weighted analyses. Future work should include attempts to identify and remove these and other potential problems before sampling.
In summary, our investigation used an efficient geocoded sampling method to demonstrate a high prevalence of active H. pylori infection in the population of a rural American Indian community. We observed a plausible association with exposure to drinking water from a public water system with a history of problems. Augmented diagnosis and treatment of symptomatic infection in this population are important for prevention of long-term consequences of chronic infection. Research in American Indian communities is needed to determine routes of transmission of H. pylori to enhance prevention efforts and reduce disease. In addition, development and validation of a conclusive test to verify the environmental presence of living H. pylori in water can enhance our understanding of the role of water in disease transmission.
ACKNOWLEDGEMENTS
We offer our sincere thanks to the clinicians, public health nurses, and community members who helped us with this investigation. This work was conducted as part of the authors' normal duties at the Centers for Disease Control and Prevention and the Indian Health Service. It required no separate funding. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention or the Indian Health Service.
DECLARATION OF INTEREST
None.







