Introduction
Graded exercise therapy (GET) or cognitive behaviour therapy (CBT) can be moderately effective for chronic fatigue syndrome (CFS) when provided by highly experienced therapists in secondary care (Whiting et al. Reference Whiting, Bagnall, Sowden, Cornell, Mulrow and Ramirez2001; NICE, 2007), but there is little evidence in primary care. Symptoms of fatigue are common (Wessely et al. Reference Wessely, Chalder, Hirsch, Wallace and Wright1997) among patients seeking care from general practitioners (GPs). When no specific cause is identified, GPs do not distinguish specifically between fatigue that does or does not meet criteria for CFS (Darbishire et al. Reference Darbishire, Ridsdale and Seed2003). This diagnosis requires 3 or 6 months' duration, 50% disability, and other symptoms (Hickie et al. Reference Hickie, Davenport, Vernon, Nisenbaum, Reeves, Hadzi-Pavlovic and Lloyd2009). In a cohort study we found that, without treatment, about 60% of patients with fatigue continued to have case-level symptoms 6 months later (Ridsdale et al. Reference Ridsdale, Evans, Jerrett, Mandalia, Osler and Vora1993). Disability associated with fatigue imposes considerable cost on patients and their families (Sabes-Figuera et al. Reference Sabes-Figuera, McCrone, Hurley, King, Donaldson and Ridsdale2010).
In prior trials, CBT, counselling and GET were associated with reduced fatigue in primary care 6 months later (Ridsdale et al. Reference Ridsdale, Godfrey, Chalder, Seed, King, Wallace and Wessely2001, Reference Ridsdale, Darbishire and Seed2004). However, these previous trials did not include a control group, so it is unclear whether the reduction was a time effect. When we compared CBT to counselling, the key predictor of a good fatigue outcome was the patients' emotional processing, including the expression, acknowledgement and acceptance of emotional distress, and specific ingredients of a particular therapy were not associated with helping patients to change (Godfrey et al. Reference Godfrey, Chalder, Ridsdale, Seed and Ogden2007). It remains unclear whether, compared to usual care, therapies delivered in primary care can reduce symptoms and, if they do, whether the benefit lasts longer than 6 months.
The aim of this trial was to compare graded exercise and counselling, both of which are readily available in general practice, to usual primary care plus a booklet on CBT (BUC). The purpose of introducing a booklet was to encourage GPs to refer, and patients to participate. A booklet has been shown to slightly enhance usual care in a community-based sample (Chalder et al. Reference Chalder, Wallace and Wessely1997). The trial objective was to evaluate changes in fatigue scores between patients in the three trial arms. Our null hypothesis was for no difference between the groups. Secondary outcomes included anxiety and depression, work/social adjustment, and patient satisfaction.
Method
Participants aged 16 to 75 years who had consulted their GP complaining of fatigue for more than 3 months and met the eligibility criteria for the trial (Table 1) were recruited between November 2003 and October 2007 from general practices in London and South East England. The eligible population was 236 000. GPs asked patients to give informed written consent for a meeting with a research associate at the practice. At this interview the trial was fully explained and written consent obtained. The trial had multi-centre ethics committee approval (MREC West Midlands MREC/02/7/71).
Table 1. Inclusion and exclusion criteria for the study

The study was a three-armed, randomized trial comparing GET or counselling (COUNS) with BUC. Patients were assessed at baseline, and at 6 and 12 months. The unit of randomization was the patient, the allocation ratio was 1:1:1, and block randomization (blocks of size 9) was used. A statistician working in a separate site performed the randomization and opaque sealed envelopes bearing sequential ID numbers were prepared, containing the randomly allocated treatment codes: BUC, GET or COUNS. The research assistant took an envelope in sequence to each baseline assessment, opened the envelope in front of the patient and explained the treatment assignment. At 6 and 12 months, each patient was sent a questionnaire and asked to complete it at home and send it to the research assistant.
Participants were offered eight sessions of individual treatment by a therapist trained in graded exercise or counselling at 2-week intervals at their local primary care practice, followed by two telephone calls from the therapist 1 month apart.
Graded exercise
GET is based on the principles of exercise prescription devised by the American College of Sports Medicine (2000) . It consisted of supervised exercise, adapted to each patient's current physical capacity, that is gradually increasing in duration according to a protocol designed for patients with CFS (Fulcher & White, Reference Fulcher and White1998). It has been evaluated in previous trials by this research group (Ridsdale et al. Reference Ridsdale, Darbishire and Seed2004). Registered physiotherapists taught participants how to measure their heart rate and provided a tailored walking exercise programme to each individual that built up from an initial 5–30 min of exercise a day. Patients were advised not to exceed the recommended duration or intensity of exercise. Exercise took the form of walking and each patient was given an instruction manual and recording sheet to monitor their progress. Eight physiotherapists saw a mean number of 10 patients for 30-min sessions.
Counselling
The counselling style used in this study followed the Rogerian client-centred, non-directive format that encouraged the patient to talk through difficulties, and reflect on their experiences and thoughts so as to understand themselves better, to arrive at alternative understandings, to uncover the links between current distress and past experience, and to provide the conditions for growth and healing (Godfrey et al. Reference Godfrey, Chalder, Ridsdale, Seed and Ogden2007). Patients were offered 50-min sessions. A senior counsellor provided supervision. Eight British Association for Counselling and Psychotherapy (BACP)-registered therapists saw a mean number of 9.5 patients each.
Usual care
Participants in the comparison arm received usual care treatment from their family doctors. To encourage practice and patient participation, this was coupled with a booklet describing causes of fatigue and providing self-help techniques based on CBT principles (Chalder, Reference Chalder1995).
Fatigue was assessed using the Chalder fatigue scale (Chalder et al. Reference Chalder, Berelowitz, Pawlikowska, Watts, Wessely, Wright and Wallace1993), an 11-item questionnaire that, when Likert scored (0, 1, 2, 3), produces a total score between 0 and 33. The primary outcome measure was the change in the Chalder fatigue score between baseline and 6 months. Secondary outcomes included the Hospital Anxiety and Depression Scale (HADS; Zigmond & Snaith, Reference Zigmond and Snaith1983) and the Work and Social Adjustment Scale (WSAS; Ware et al. Reference Ware, Sherbourne, Davies, Stewart and Ware1992), measuring degree of functional impairment in work, home, private and leisure (not at all impaired=0; very severely impaired=8). Patient satisfaction with treatment was recorded at 6 and 12 months using seven categories, but given the sparse cross-tabulations by therapy, the categories were collapsed into three (very/moderately/slightly satisfied; neither; very/moderately/slightly dissatisfied).
At baseline, self-reported rating using the European Questionnaire measuring health-related quality of life in five dimensions with UK weights attached (EQ-5D; Dolan et al. Reference Dolan, Gudex, Kind and Williams1995) was measured, in addition to patient's preferences for treatment and other characteristics, which were measured serially.
Statistical analysis
We based our power calculation on previous studies where the mean changes in fatigue score at 6 months were approximately 5 for usual medical care, 10 for GET and 9 for counselling (Ridsdale et al. Reference Ridsdale, Evans, Jerrett, Mandalia, Osler and Vora1993, Reference Ridsdale, Godfrey, Chalder, Seed, King, Wallace and Wessely2001, Reference Ridsdale, Darbishire and Seed2004). In this trial, we aimed to detect a difference of 4 units (standard deviation of 5.5) in the mean change fatigue score between usual care and either of the active interventions (GET or COUNS), at the 5% (two-tailed) level of significance and 80% power, for which 30 patients per arm were required. With 15 patients, on average, for each therapist and an intra-therapist correlation of 5% (design effect=1.7), a total of 153 patients across 18 therapists were required. Assuming a drop-out rate of 30%, a total of 225 patients were sought.
An intention-to-treat (ITT) approach was used. The principal analysis consisted of mixed linear, ordinal and logistic regressions for the continuous, ordinal and binary outcomes respectively. As the study is a randomized trial of moderately large sample size and with no anticipated confounders, the unadjusted comparison of the groups is presented for both the primary and the secondary analysis. We nevertheless checked all the potential prognostic variables assessed in the study: demographic, social and clinical baseline characteristics (as shown in Tables 2 and 3). The multiple regressions included only those variables that were significant at <0.25 in the univariate models. Final significance in the multiple regressions was judged at the usual 5% level. A binary variable was created to indicate whether a patient had been allocated to a therapy that would not have been of their choice. We explored the effect of this on outcome and adherence.
Table 2. Demographic and social characteristics of each group at baseline
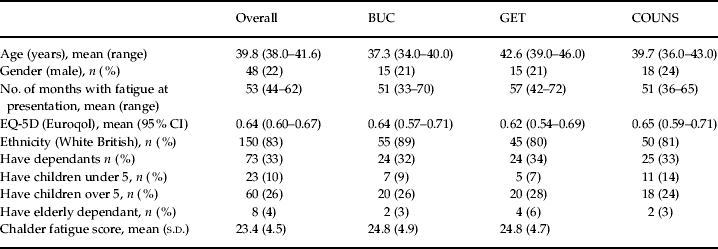
EQ-5D, European Quality of Life Questionnaire – 5 Dimensions; BUC, usual care plus a cognitive behaviour therapy (CBT) booklet; GET, graded exercise therapy; COUNS, counselling; CI, confidence interval; s.d., standard deviation.
No significant difference between groups was observed.
Table 3. Observed outcomes by therapy

BUC, Usual care plus a cognitive behaviour therapy (CBT) booklet; GET, graded exercise therapy; COUNS, counselling; HADS, Hospital Anxiety and Depression Scale; WSAS, Work and Social Adjustment Scale; OR, odds ratio; CI, confidence interval; s.d., standard deviation.
Classification of missing data, using missing at random (MAR) analysis, was inferred by modelling the likelihood of missingness using a logistic regression model and we modelled the outcome using both complete case and multiple imputations for the missing values of the independent and dependent variables. The multiple imputation algorithm generated 20 datasets assuming a greater than 95% fraction of missing information, 50 times per data set, and the imputation models were based on results from complete case analyses. Moreover, to account for variables found to be related to missingness in the MAR analysis, the variables ‘age’ and ‘compliance status’ were also included in the imputation models. Analyses of the 20 datasets was conducted in accordance with Rubin's rules (Rubin, Reference Rubin1987). In addition, using all available data, estimates of means for the complier and non-complier groups within each therapy are provided. The data analysis was conducted in Stata version 11 (Stata Corporation, USA).
Results
GPs referred 324 patients with fatigue to the study, and 222 reached baseline assessment (Fig. 1). Adherence to the allocated therapy was measured by the number of therapy sessions attended. These ranged from zero to eight, with a mean of 5.8 (s.d.=3) attended for GET and 5.9 (s.d.=2.8) for COUNS. The 25th, 50th (median) and 75th percentiles were 3-8-8 for GET and 4-8-8 for COUNS. Age was the only factor significantly associated with compliance: patients aged over 35 years were 2.6 times as likely to attend all eight sessions compared to younger patients.
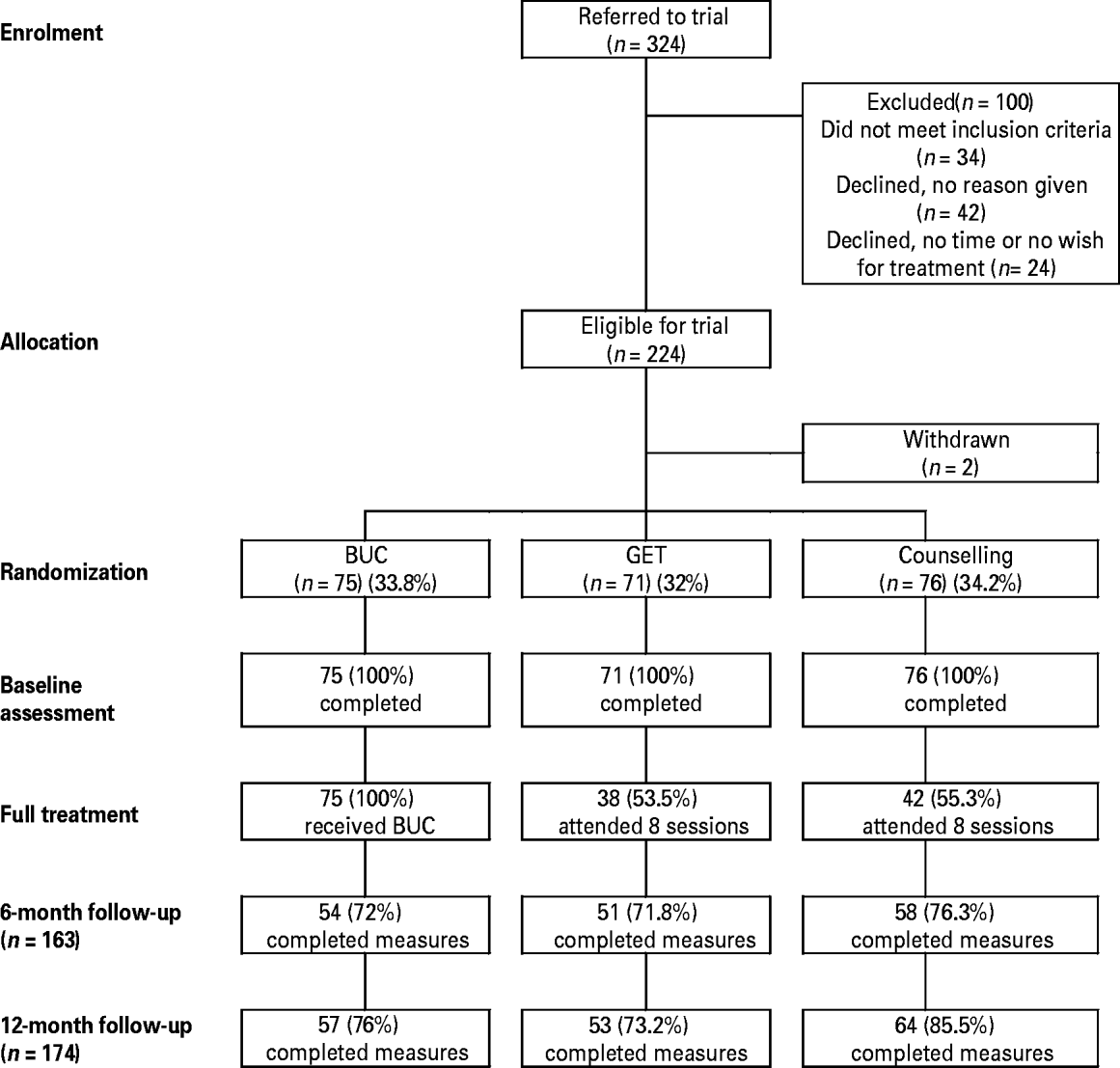
Fig. 1. The flow of participants. BUC, Usual care plus a cognitive behaviour therapy (CBT) booklet; GET, graded exercise therapy.
The three groups were balanced by sociodemographic characteristics and baseline health outcome measures (Table 2). Table 3 illustrates primary and secondary outcomes at baseline, 6 and 12 months. A total of 222 patients were assessed at baseline, and 163 and 174 patients were assessed at 6 and 12 months respectively. The distribution of missing data was not significantly associated with the allocated group for either the 6-month (p=0.78) or the 12-month (p=0.36) assessment. There was a significant association between older age and missing data on fatigue score at the 12-month assessment [odds ratio (OR) 0.97, 95% confidence interval (CI) 0.94–1.0, p=0.02].
Fatigue scale
There were 559 observations in 222 patients recruited by 19 therapists. There was no significant therapist effect. A mixed multiple linear regression on the complete data revealed a significant time effect: there was a mean improvement in the Chalder fatigue scale of 9.2 (mean=−9.2, 95% CI −10.3 to −8.1, p<0.0001) between baseline and the 6-month follow-up and a non-significant mean improvement of 0.94 (mean=−0.94, 95% CI −1.9 to 0.03, p=0.06) between the 6-month and the 12-month follow-up. The mean improvement between baseline and 12 months was 10.1 (mean=−10.1, 95% CI −11.2 to −9.1, p=0.0004). None of the potential prognostic variables tested had a significant effect on outcome. The time by group interaction was not significant, indicating that the reduction in fatigue at either 6 or 12 months was similar for the three groups. The mean improvement at 6 months was 8.1 (95% CI 6.6–10.4) for BUC, 10.1 (95% CI 7.5–12.6) for GET and 8.6 (95% CI 6.5–10.8 ) for COUNS. The change (reduction) at 12 months was −10.2 (95% CI −12 to −8.3) for BUC, −10.7 (95% CI −12.8 to −8.6) for GET and −9.2 (95% CI −11.2 to −7.2) for COUNS.
There was no significant difference in the overall mean level of the Chalder fatigue scale between BUC and GET (mean=−1.13, 95% CI −4.2 to 1.9, p=0.46) or between BUC and COUNS (mean=0.36, 95% CI −2.6 to 3.3, p=0.81) at 6 months (Table 3). Similarly, there was no significant difference in means on the Chalder fatigue scale between BUC and GET (mean=−0.06, 95% CI −1.8 to 1.6, p=0.94) or between BUC and COUNS (mean=0.99, 95% CI −0.7 to 2.6, p=0.24) at 12 months.
There were data on preference for treatment for 168 patients. The effect of this variable was not statistically significant on the outcome of fatigue total score. Preference did not show any association with adherence (attending to all eight sessions of therapy) status.
Anxiety and depression and work and social adjustment
All three groups experienced a similar reduction in HADS depression and anxiety scores between the baseline and 6-month assessments. No significant differences were identified between BUC and GET and between BUC and COUNS on the WSAS (Table 3).
Dissatisfaction with care
Over half of all patients reported dissatisfaction with care at 6 months, with no significant difference between the three arms (Table 3). An ordinal logistic regression showed that each extra month in the duration of fatigue reported at baseline increased the odds of a higher level of dissatisfaction by 1% (OR 1.01, 95% CI 0.9–1.004, p=0.01). Dissatisfaction increased for participants allocated to BUC between the 6-month and 12-month follow-up, whereas satisfaction increased for the participants receiving GET and COUNS. In relation to the BUC group, the OR of dissatisfaction at the 12-month assessment was significantly less for the GET (OR 0.11, 95% CI 0.02–0.54, p=0.01) and COUNS groups (OR 0.13, 95% CI 0.03–0.53, p=0.004).
Discussion
Following entry to the trial for chronic fatigue, the Chalder fatigue score declined in all three groups over 6 months (BUC −8.1, GET −10.1, COUNS −8.6). The mean improvement in fatigue scores after 6 months did not differ significantly between patients receiving BUC and those receiving GET (−1.13, 95% CI −4.2 to 1.19) or COUNS (0.36, 95% CI −2.6 to 3.3). However, at 12 months, groups allocated to GET and counselling were less dissatisfied than those allocated to usual care, suggesting that patients valued therapy.
Our results are conclusively negative with CIs for the comparison of change scores well within the minimum difference of interest assumed when choosing the sample size. Our standard deviation estimates were also confirmed in the trial data. There was good compliance with allocated therapy, with patients taking up six to eight sessions. Our findings suggest that many patients improve substantially in the first 6 months. This factor, time, is likely to explain the improvement suggested in prior trials that used evidence from cohorts as comparators rather than randomized control groups (Ridsdale et al. Reference Ridsdale, Evans, Jerrett, Mandalia, Osler and Vora1993, Reference Ridsdale, Godfrey, Chalder, Seed, King, Wallace and Wessely2001, Reference Ridsdale, Darbishire and Seed2004). GPs manage the majority of patients with fatigue. This evidence derived from primary care is more likely to be generalizable to primary care than evidence derived by therapists working in specialist care with referred CFS patients. A further strength is that we found little evidence of variation in outcome between therapists.
Wearden et al. (Reference Wearden, Dowrick, Chew-Graham, Bentall, Morriss, Peters, Riste, Richardson, Lovell and Dunn2010) published a trial from primary care in which they recruited only patients with more severe CFS. Therapies consisted of pragmatic rehabilitation and supportive listening, implemented by nurses with additional training rather than the physiotherapists and counsellors working in our trial. The nurse interventions also had non-significant effects on fatigue at the 1-year follow-up.
We offered two sessions and two telephone calls more than in our prior trials of six sessions of GET and counselling (Ridsdale et al. Reference Ridsdale, Godfrey, Chalder, Seed, King, Wallace and Wessely2001, Reference Ridsdale, Darbishire and Seed2004). Several explanations are compatible with the finding of a lack of significant difference in outcome, in particular that greater than expected improvement occurred in the usual care group, and that less improvement occurred in the treatment groups even though up to eight sessions were provided. It is already known that a CBT booklet is itself more effective than usual care (Chalder et al. Reference Chalder, Wallace and Wessely1997). A CBT booklet co-intervention with the usual care group may have added slightly to the effectiveness of usual medical care. Most therapists working in usual National Health Service (NHS) practice are less expert, do not see sufficient case volume, or give a therapy long enough to achieve the effect demonstrated in tertiary care trials. In the study by Deale et al. (Reference Deale, Chalder, Marks and Wessely1997), delivering an average of 15 h of CBT to participants with CFS achieved a 6-point reduction in mean fatigue (binary scored 0011). When CBT was delivered by many NHS CBT therapists in the same centre, but outside the trial context, Quarmby et al. (Reference Quarmby, Rimes, Deale, Wessely and Chalder2007) found that the fatigue score declined by only 3.5 (binary) points. This is less than the mean 4.6 (binary scored) decline we found in our trial for the BUC group.
A recent study by White et al. (Reference White, Goldsmith, Johnson, Potts, Walwyn, DeCesare, Baber, Burgess, Clark, Cox, Bavinton, Angus, Murphy, Murphy, O'Dowd, Wilks, McCrone, Chalder and Sharpe2011) of patients with CFS found a moderate difference (mean 3.2 points on a Likert scale) between a longer course (up to 15 sessions) of GET plus usual specialist care after 1 year. Chronic fatigue is a remitting and relapsing condition clinically, and it may be that a longer course of treatment or a booster dose is needed to achieve sustained improvement (Deale et al. Reference Deale, Chalder, Marks and Wessely1997; Fulcher & White, Reference Fulcher and White1997).
The results of the current study do not support early implementation of a short course of either GET or counselling for chronic fatigue in primary care. However, participants tended to be less dissatisfied after graded exercise and counselling. Hitherto, patients with chronic fatigue have expressed dissatisfaction with management (NICE, 2007), and this is supported by our evidence. We found patients who had experienced prolonged fatigue symptoms before the trial were more likely to report dissatisfaction. Dissatisfaction sometimes undermines the doctor–patient relationship (Bowie, Reference Bowie2008). Our quantitative and qualitative studies suggest that patients are more satisfied with seeing a therapist in addition to usual primary care, and qualitative data show that, irrespective of changes in fatigue, both the relationship and time spent with therapists were valued (Godfrey et al., unpublished observations). Satisfaction with primary care is a performance indicator, and eligible for remuneration (Department of Health, 2009). We believe that people appreciate being seen by someone for six to eight sessions of therapy. It may be that time and personal attention are important process variables. It seems likely that, when not offered a therapeutic intervention, dissatisfaction persists or increases. In the absence of evidence for efficacy, GPs can at the least provide usual advice plus written self-help information on managing chronic fatigue, as a form of health promotion in primary care. In a separate paper we report the cost of therapy, and show that GET is less expensive to provide than counselling (Sabes-Figuera et al., unpublished observations).
From the current evidence, we propose that after assessment of patients who present with fatigue in primary care, doctors offer to reassess them in 6 months. If fatigue symptoms persist, the practitioner and patient may discuss further therapy options.
Acknowledgements
We thank A. Passalacqua, S. Spector, A. Wearden, R. Jones, and our anonymous referees for advice, and the Wellcome Trust for funding (068474/Z/02/Z). We also thank the GPs and practices that participated at the study: Brigstock Medical Centre, Canbury Medical Centre, Cheam Family Practice, Crown Dale Medical Centre, Dr Laurence & Partners (West Byfleet Health Centre), Elizabeth House Surgery, Fairhill Medical Practice, Hamsey Green Surgery, Hillview Medical Centre, Lambeth Walk Group Practice, Lavender Hill Group Practice, Morden Hill Surgery, Parishes Bridge (West Byfleet Health Centre), Partkside Group Practice, Paxton Green Health Centre, Selsdon Park Practice, South Lewisham Group Practice, Tadworth Medical Centre, The Church Lane Practice, The Hurley Clinic, The Jenner Practice, The Nunhead Surgery, The Oaklands Practice, The Surgery, Lower Addiscombe Road, The Vanbrugh Group Practice 2000, The Woodcote Group Practice, Waterloo Health Centre, Wells Park, and Wrythe Green Surgery.
Declaration of Interest
None.








